What is the Asthma Treatment Market Size?
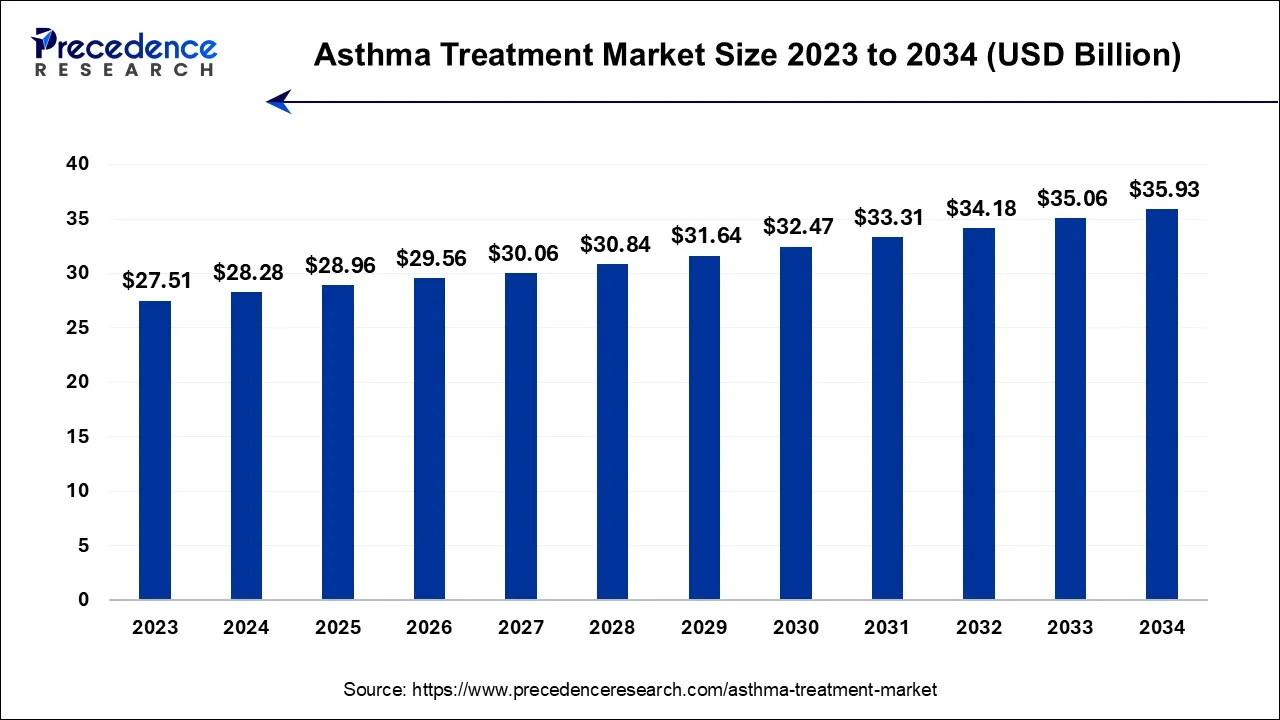
The global asthma treatment market size is valued at USD 28.96 billion in 2025 and is predicted to increase from USD 29.56 billion in 2026 to approximately USD 35.93 billion by 2034, expanding at a CAGR of 2.42% over the forecast period from 2025 to 2034. The rising prevalence of asthma due to increasing levels of pollution is expected to augment the growth of the market.
Asthma Treatment Market Key Takeaways
- In terms of revenue, the market is valued at $28.96 billion in 2025.
- It is projected to reach $35.93 billion by 2034.
- The market is expected to grow at a CAGR of 2.42% from 2025 to 2034.
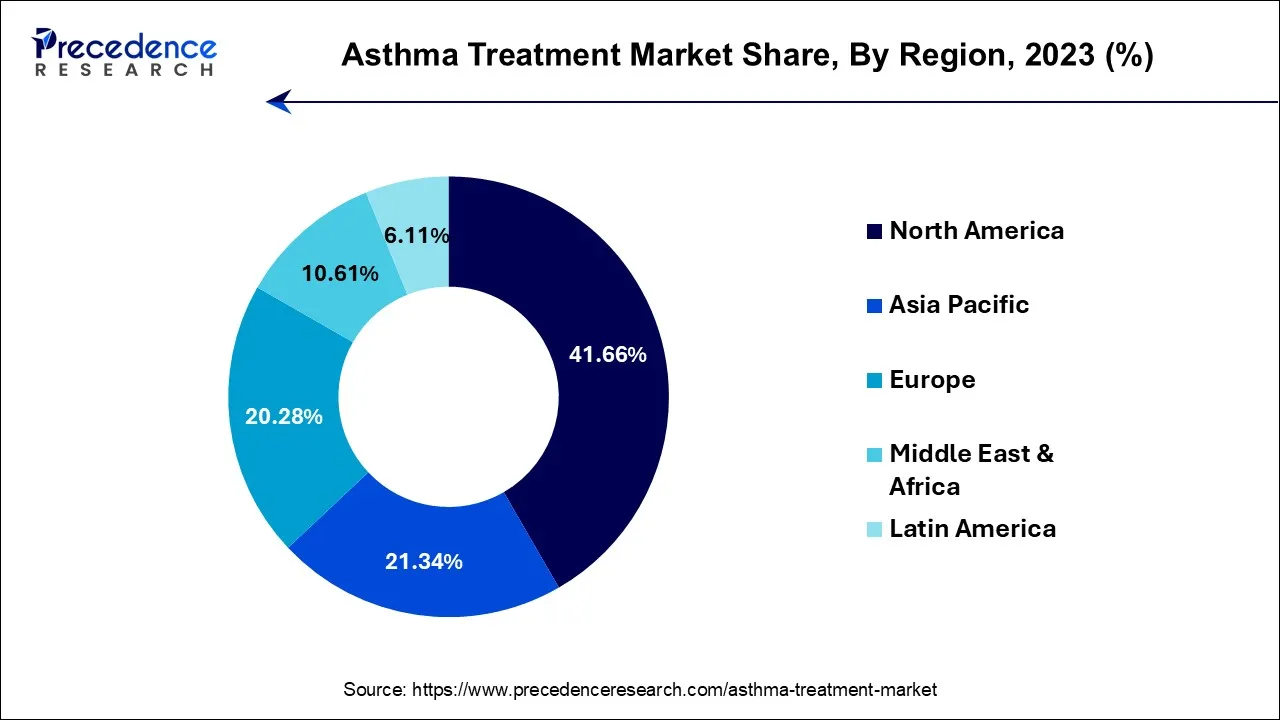
- North America led the global market with the highest market share of 41.66% in 2024.
- By medication, the long-term control medication segment registered a maximum market share of 59.86% in 2024.
- By route of administration, the inhalers segment captured the biggest revenue share of 66.56% in 2024.
- By adjunct therapy, the LABA (long-acting beta antagonists) segment has held the largest market share of 23.52% in 2024.
- By distribution channel, the retail pharmacies & drug stores segment is estimated to hold the highest market share of 42.31% in 2024.
What is an asthma treatment?
There has been a strong relation established between psychological disorders and its impact on asthma. The increasing occurrence of psychological disorders is expected to trigger asthma in patients, especially for those whose ailment in severely undertreated. This is expected to drive the global market growth. However, studies have found that there is a severe lack of adherence to asthma treatment, especially, in underdeveloped countries and an array of unmet needs. These factors are expected to hamper the market growth. Nonetheless, biologics for asthma management are expected to open new growth opportunities.
The global asthma treatment market is consolidated with the top 5 companies accounting for 75 percent of the total market share in 2020. The global market was dominated by GSK, AstraZeneca, Sanofi-Aventis, Boehringer Ingelheim, and Teva. The corporations have been concentrating their efforts on product development and regulatory approval. In addition, the companies sell asthma medications as well as accessories such as inhalers.
What are the Key Impacts of AI on the Asthma Treatment Market?
Asthma treatment is becoming personalized and precise due to the impact of artificial intelligence (AI). AI uses data gained from smart inhalers and applications to help doctors predict asthma attacks in patients much earlier. AI has also educated clinicians' ability to capture a person's ability to adhere to their treatment plan through monitoring and recommends dosage adjustments where needed. Moreover, pharmaceutical companies have begun to utilize AI to accelerate drug discovery, to improve the patient experience and route for clinical trials, and to ultimately revolutionize prescription medications with fewer side effects for the asthmatic patient.
Market Outlook:
- Industry Growth Overview: The asthma treatment market is expected to expand rapidly between 2025 and 2030 due to rising asthma diagnosis rates, higher asthma incidence rates, and increased user acceptance of combination therapies. The majority of growth will be attributed to the advances in biologics and smart inhaler technologies, primarily in North America and the Asia Pacific, as access to healthcare and awareness of inhalers continue to rapidly develop in those regions.
- Sustainability Trends: The market is pursuing inhalers made of sustainable materials and recyclable packaging to reduce its carbon footprint. Companies like GSK and AstraZeneca are investing in propellant-free inhalers and methods of production designed to preserve raw materials to align with global sustainability objectives and increasingly stringent EU emission targets.
- Global Expansion: Top global pharmaceutical companies are expanding their respiratory medications in emerging markets (e.g., India, Brazil, and Indonesia) where there are large populations of patients and healthcare initiatives that promote early diagnosis and treatment of asthma.
- Major Investors: Institutional investors and venture funds are increasingly backing up respiratory biotech firms developing next-generation biologics and AI-powered inhaler systems. Firms like BlackRock and Novo Holdings are actively funding companies focused on severe asthma therapies and precision medicine.
- Startup Ecosystem: Startups are innovating digital asthma management, wearable sensors, and drug-delivery devices. Firms such as Propeller Health and FindAir are gaining traction with connected inhalers and real-time symptom tracking, drawing strong VC interest for improving patient adherence and outcomes.
Market Scope
| Report Coverage | Details |
| Market Size by 2034 | USD 35.93 Billion |
| Market Size in 2025 | USD 28.96 Billion |
| Market Size in 2024 | USD 28.28 Billion |
| Market Growth Rate from 2025 to 2034 | CAGR of 2.42% |
| Fastest Growing Region | North America |
| Base Year | 2024 |
| Forecast Period | 2025 to 2034 |
| Segments Covered | Medication, Route of Administration, Adjunct Therapy, Distribution Channel, and Region |
| Regions Covered | North America, Europe, Asia-Pacific, Latin America, and Middle East & Africa |
Market Dynamics
Drivers
Increasing air pollution triggering asthma cases
- Asthma is a chronic respiratory condition marked by fluctuating airflow restriction, bronchial hyper responsiveness, and inflammation of the airways. Air pollution appears to have a negative impact on asthma outcomes in both adults and children, according to research. Air pollution from traffic, nitrogen dioxide, and secondhand smoking (SHS) are all substantial risk factors for the development of asthma in children. Nonetheless, a link between air pollution and adult asthma development has yet to be demonstrated. Asthma symptoms, exacerbations, and decreased lung function can all be triggered by exposure to outside pollution.
- For instance, in the US, Exposure to air pollution has long been associated with asthma, a serious and life-threatening chronic respiratory condition that impacts the quality of life of more than 23 million Americans. Asthma symptoms can be aggravated and asthma attacks might be triggered by air pollution. Children with asthma, which affects an estimated six million children in the United States, are particularly vulnerable to pollution.
Air pollution may impact DNA associated with asthma
- A new study financed by the Environmental Protection Agency (EPA) sheds light on the link between air pollution and asthma. While experts aren't sure why air pollution causes asthma, evidence suggests that it suppresses genes that control the immune system's ability to distinguish between an allergen and a hazardous foreign substance like a virus or bacteria. The immune system then goes into overdrive, triggering an inflammatory reaction regardless of whether the drug is toxic, resulting in asthma.
- Each of these asthma research has improved our understanding of childhood asthma and supplied crucial information to the Environmental Protection Agency (EPA) that may be used to protect human health and the environment.
Rising prevalence of psychological disorders to impact asthma in patients
- Asthma has been recognized as a disorder in which psychological elements play a significant role since the turn of the twentieth century. Clinicians understand that emotional stress can trigger or exacerbate asthma and that a patient's mental health can impair asthma control by influencing symptom presentation and treatment adherence. As a result, there is a bi-directional link between asthma and psychological issues.
- Asthmatics have been associated with periods of heightened emotionality, and asthma exacerbations have been linked to periods of heightened emotionality. Depressive disorders are likely to be more common among people with asthma than in the general population, according to a variety of prevalence estimates, some of which reach 40%. Remarkably, there is a link between depression and asthma in both families and individuals; familial studies imply that the prevalence of one condition is higher in the family members of index cases with the other. Patients with bipolar affective disorders tend to have a higher chance of acquiring IgE-mediated allergy diseases, such as asthma than the general population. Anxiety disorders also have an elevated prevalence in asthma, affecting up to one-third of asthmatic children and adolescents, as well as 24% of asthmatic adults.
- Unfortunately, ambiguous disease criteria, inconsistencies in nomenclature, limited samples, and an emphasis on outpatient or inpatient populations rather than the community complicate the research on the frequency of psychological and mental disorders in asthmatics. The World Mental Health Survey addresses some of these methodological issues by providing standardized data for 17 nations throughout the world.
Exposure to coarse particulate matter linked with asthma in children
- Researchers theorized that this was because younger children spend more time outside than older children and their respiratory systems are still maturing. This is the first study to look at the long-term impact of coarse PM on asthma in a countrywide sample of children in the United States.
- This conclusion is relevant because exposure to fine particulate matter (PM2.5) has been linked to the development of asthma and other respiratory and cardiovascular disorders in the past. Because the greater particle size restricts penetration deep into the lungs, coarse particulate matter was assumed to be less hazardous. Coarse PM, on the other hand, can settle in the lungs, and current evidence suggests that short-term exposure is linked to cardiovascular and respiratory problems.
- Between 2009 and 2010, researchers looked at a dataset of approximately eight million children aged 5 to 20 who were enrolled in Medicaid in 34 states. They discovered that coarse PM exposure was linked to an increase in asthma diagnoses, hospitalizations, and emergency department visits, with children aged 11 and under is the most vulnerable to the negative health impacts of coarse PM exposure.
Opportunity
Biologics for asthma management to open new market opportunities
A biologic is a drug derived from the cells of a live organism, such as bacteria or mice, then tailored to target specific molecules in humans. Antibodies, inflammatory chemicals, and cell receptors are the targets for asthma. Biologics attempt to disrupt the processes that contribute to inflammation, which causes asthma symptoms, by targeting these molecules.
Patients who continue to experience symptoms despite taking normal daily controller drugs are given a biologic. Symptoms of poorly controlled asthma include recurrent hospital admissions, emergency room visits, or the need for oral steroids for exacerbations; waking up at night with difficulty breathing; requiring a fast-acting reliever medication, such as albuterol, several times a day or week; and requiring a fast-acting reliever medication, such as albuterol, several times a day or week. Before prescribing a biologic, clinicians should ensure that the patient is taking all of their other controller medications as prescribed, avoiding any potential triggers, and treating any other medical illnesses that may be exacerbating their asthma.
The main advantage of biologics has been a reduction in the number of asthma exacerbations, which includes ER visits, hospitalizations, and the need for oral steroids. Reduced asthma symptoms, lower dosages of other controller medications, and fewer missed school and work days are among the other advantages. Biologics have been found to improve asthmatic patients' quality of life. Some biologics have been reported to help people with severe asthma improve their lung function.
Currently, five biologics for asthma are approved: omalizumab, mepolizumab, reslizumab, benralizumab, and dupilumab, with numerous more in the works. Omalizumab is an antibody that targets IgE allergy antibodies. Mepolizumab, reslizumab, and benralizumab all target eosinophils, a type of cell that plays a role in allergic inflammation. Dupilumab is a monoclonal antibody that targets a receptor for two molecules that cause allergic inflammation. To determine which biologic might be best for treating asthma, a doctor will obtain screening tests such as blood work or environmental allergen skin prick testing. Except for reslizumab, omalizumab is approved for patients as young as six years old. All other biologics, except for reslizumab, are approved for individuals as young as twelve years old. Adults aged 18 and up are permitted to use Reslizumab.
Biologics have been proved in trials to be quite safe and have little side-effects. Although biologics are more expensive than other controller drugs, the price is likely to drop as demand grows, the introduction of new biologics, and manufacturing economies of scale are realized.
Medication Insights
Based on medication, the long-term control medication segment accounted largest revenue share of 59.86% in 2023. Increasing prevalence of asthma is expected to drive the growth of this sector during the forecast period. The majority of people with asthma require one or more long-term controller medicines that must be taken daily, regardless of their symptoms or lack thereof. Regardless of their symptoms or lack thereof, the majority of persons with asthma require one or more long-term controller drugs that must be taken daily. Asthma exacerbations are prevented by a controller medication, which reduces chronic airway inflammation over time. The most prevalent type of asthma management medication is long-acting inhalers. They normally take a few days to a few weeks to start working, but you should notice that you need your rescue prescription less and less after that.
The quick-relief inhalers, also known as rescue inhalers, are short-term drugs that are used to treat acute asthma symptoms such as wheezing, chest tightness, shortness of breath, and coughing. A quick-relief inhaler should be carried by everyone with asthma. It could be the only treatment for:
- Asthma attacks that aren't severe. Intermittent asthma refers to asthma attacks that occur twice a week or fewer, with overnight symptoms occurring no more than twice a month.
- Asthma is brought on by exercise. Physical exercise triggers this form of asthma.
Global Asthma Treatment Market, By Medication, 2020-2023 (USD Million)
| By Medication | 2020 | 2021 | 2022 | 2023 |
| Quick-relief medication | 9,792.80 | 10,292.20 | 10,681.80 | 11,044.40 |
| Long-term control medication | 14,796.40 | 15,482.20 | 15,997.30 | 16,467.10 |
Route of Administration Insights
Asthma inhalers accounted for the largest market share of over 66.56% in 2024 and the trend is expected to continue during the forecast year. Asthma inhalers are the most common and effective way to get asthma medication into your lungs. However, the demand for prefilled syringe/vials is expected to outdo every segment during the forecast period.
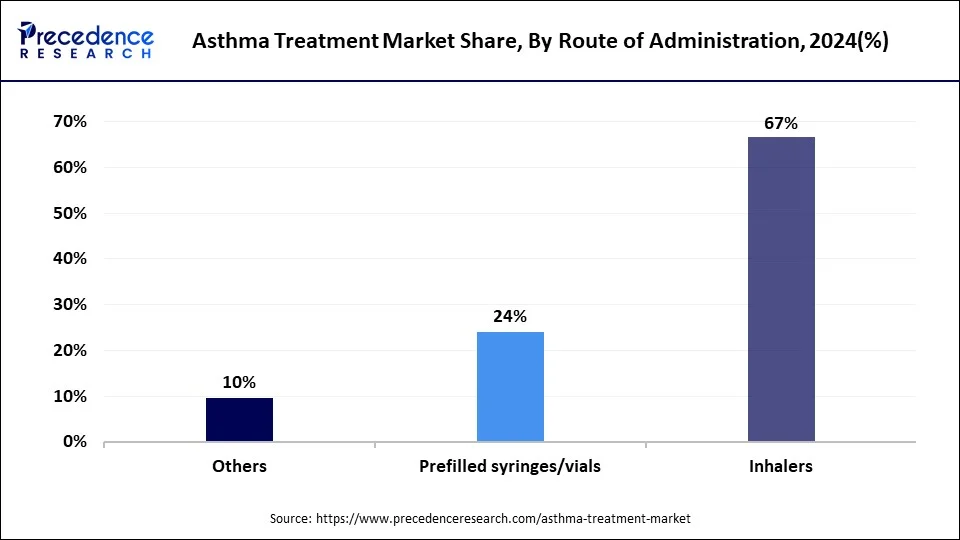
The safety of prefilled syringes is expected to drive their demand. Additionally, the global spread of COVID-19 is pushing up demand for prefilled syringes and vials. Hospital pharmacies and retail pharmacies & drugstores together dominated the global asthma treatment market in 2020. However, the demand from online pharmacies has increased tremendously due to the lockdown across the world.
Global Asthma Treatment Market, By Route of Administration, 2020-2023 (USD Million)
| By Route of Administration | 2020 | 2021 | 2022 | 2023 |
| Inhalers | 17,279.70 | 17,794.00 | 18,088.70 | 18,313.00 |
| Prefilled syringes/vials | 4,838.20 | 5,436.50 | 6,005.10 | 6,582.10 |
| Others | 2,471.20 | 2,543.90 | 2,585.20 | 2,616.30 |
Adjunct Therapy Insights
Based on adjunct therapy, the LABA (long-acting beta antagonists) segment garnered a market share of over 23.52% in 2024. This segments was valued at USD 6,469.5 million in 2023 and is projected to reach a CAGR of 3.26% during the forecast period 2024 to 2034.
Long-acting beta-agonists (LABAs) are bronchodilators with a 12-hour or longer duration of action. They are not used to treat acute asthma or asthma exacerbations and are only used as an add-on medication for symptom prevention. LABAs should only be used in combination with inhaled steroids, and they should only be used when a low dose of inhaled corticosteroids isn't enough to control symptoms.
Long-term asthma control is achieved with combination asthma inhalers. They combine two inhaled drugs: a corticosteroid and a long-acting beta-agonist (LABA). LABAs are bronchodilators that expand and open constricted airways to allow free passage of air. Corticosteroids suppress inflammation, while LABAs are bronchodilators that widen and open constricted airways to allow free flow of air. These drugs, when taken together, can reduce airway hyper responsiveness and help prevent asthma attacks.
Distribution Channel Insights
Based on the Distribution Channel, the retail pharmacies & drug stores segment accounted largest revenue share 42.31% in 2024. Online pharmacies segment held the revenue share of 25.56% in 2023. The Internet has unquestionably had an impact on every part of our lives, including how we work, learn, and purchase. The recent global pandemic of COVID-19 has only strengthened the position of digital commerce, which has experienced rapid and sustained growth. The second COVID-19 wave has increased sales by 25-65% for online pharmacies in India. Similarly, While Czech and Slovak's citizens are no strangers to online shopping (70 percent of Czechs have made at least one online purchase in their lives and nearly 59 percent in the last 12 months; in Slovakia, 63 percent of citizens aged 16 to 74 made an online purchase in the last year), purchasing health-related products has been relatively limited in the Czech Republic. The sales of online pharmacies for asthma products are expected to increase tremendously over the next few years due to the continued prevalence of COVID-19. Asthma patients prefer ordering medications online due to the fear of being exposed to the virus as well as the dread of insufficient availability.
The hospital pharmacies segment was valued at USD 8,839.4 million in 2023 and is projected to reach a CAGR of 1.67% during the forecast period 2024 to 2034. Hospital pharmacy sales have been impacted by the COVID-19 pandemic. In certain cases, patients with controlled asthma visited hospital pharmacies at a lower frequency than where asthma was not controlled. Furthermore, breathing complications associated with coronavirus patients boosted hospital pharmacy sales.
Global Asthma Treatment Market, By Distribution Channel, 2020-2023 (USD Million)
| By Distribution Channel | 2020 | 2021 | 2022 | 2023 |
| Online pharmacies | 6,165.10 | 6,503.70 | 6,775.00 | 7,030.70 |
| Hospital pharmacies | 8,114.40 | 8,430.80 | 8,649.40 | 8,839.40 |
| Retail pharmacies & drug stores | 10,309.70 | 10,839.90 | 11,254.70 | 11,641.30 |
U.S. Asthma Treatment Market Size and Growth 2025 to 2034
The U.S. asthma treatment market size accounted for USD 11.23 billion in 2025 and is projected to be worth around USD 13.10 billion by 2034, poised to grow at a CAGR of 1.73% from 2025 to 2034.
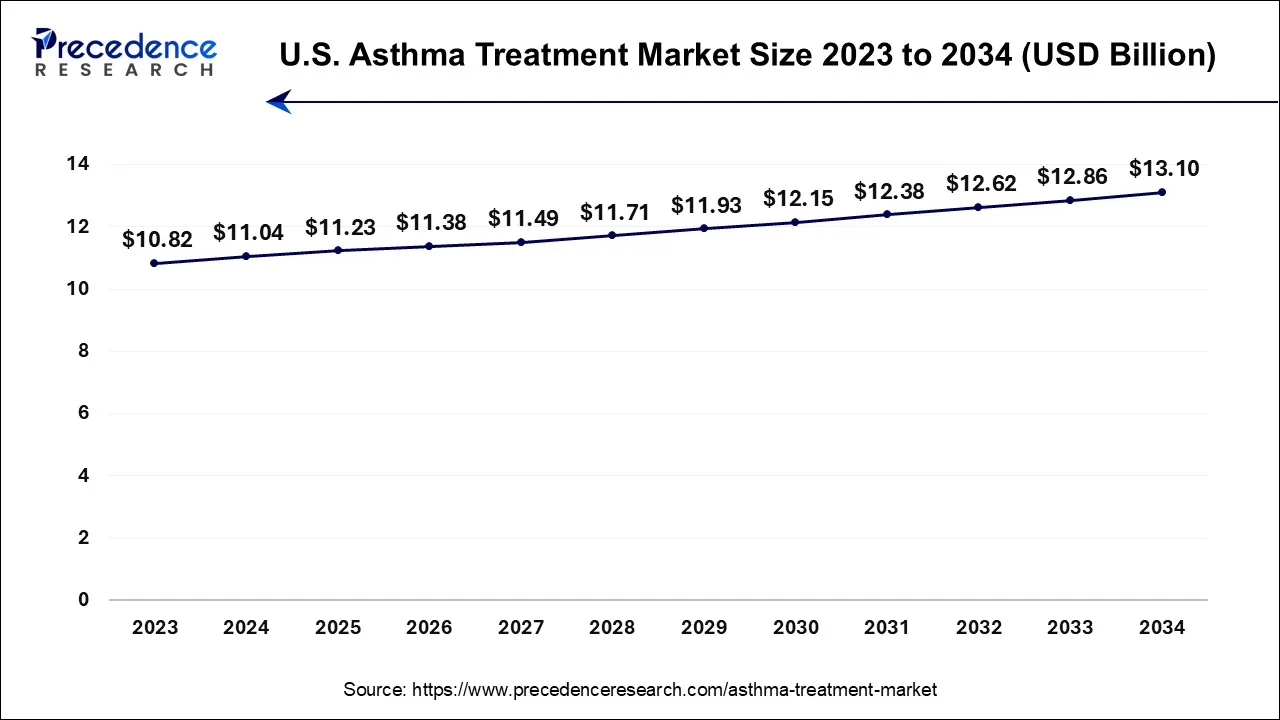
U.S.
In 2018, 24.8 million Americans, or 7.7% of the population, had ever been diagnosed with asthma and reported that they still had asthma. Current asthma prevalence rates increased at a statistically significant average rate of 0.1 points per year from 2001 to 2010. Between 2010 and 2018, the average annual change was statistically insignificantly different and remained flat.
Asthma is linked to a variety of factors, including gender, race, ethnicity, and socioeconomic level, with males experiencing the condition at a higher rate than girls in childhood. In maturity, the trend reverses, with more women than males suffering from asthma. Race and ethnicity have a substantial impact on prevalence rates. When compared to any other racial or ethnic group in the United States, Puerto Ricans have the highest rate of asthma prevalence. In addition, black Americans are diagnosed with asthma at a higher rate than white Americans.
Canada
Asthma is a chronic lung illness that causes airflow restriction in the lungs, making breathing difficult for almost 3.8 million Canadians. It is Canada's third most frequent chronic condition. Many environmental variables provoke asthma symptoms, which include shortness of breath, chest tightness, wheezing, and coughing, all of which narrows the airways (bronchial tubes). Every day, almost 300 Canadians are diagnosed with asthma, and around 250 Canadians die as a result of an asthma attack.
For good asthma management and symptom control, timely access to quality health care, treatment, and education is critical. Despite this, over half of respondents (44%) said their current drug coverage is insufficient, and 24% said they have avoided filling a prescription because they couldn't afford it. Although family doctors, pediatricians, and emergency room doctors are more likely to diagnose asthma (63%) than asthma specialists (23%), the primary source of care and management for those living with asthma remains a family doctor or pediatrician (52%) followed by an asthma specialist (23%). Access issues, wait times to see a specialist, a lack of information and education on managing asthma, as well as referrals and follow-up following emergency care, are all top needs in our community. In a pandemic, this can be much more difficult and concerning, given the influence that heightened safety procedures, as well as the worry and dread associated with COVID-19, have on patients seeking treatment.
The poll also revealed that people's perceptions of asthma control differ significantly from the clinical definition of control. Even during a worldwide pandemic, this can be a substantial impediment to optimizing asthma management. Although 83 percent of respondents believe their asthma is moderate to very well controlled (up from 63 percent during COVID-19), 59 percent report difficulty sleeping as a result of asthma symptoms, and 71 percent avoid exercise or physical activities as a result of asthma symptoms. Improved access to affordable drugs, reliable testing, and diagnosis, and early diagnosis and care can all help people with asthma live a better life.
- The Europe region was valued at USD 5,579.7 million in 2023 and is expected to reach a CAGR of 3.53% over the forecast period.
- The Latin America region was valued at USD 1,681.7 million in 2023 and is projected to hit a CAGR of 3.34% over the forecast period.
Asia Pacific is expected to grow significantly in the asthma treatment market during the forecast period. The growing occurrences of asthma in the Asia Pacific are increasing the need for asthma treatment approaches. The growing pollution is also leading to a rise in the asthma patients. Thus, the demand for new asthma treatment approaches, such as biologics or inhalers, is increasing.
At the same time, developing healthcare is focusing on various strategies to spread awareness as well as for early diagnosis and treatment options. Additionally, the use of generic asthma medications is also driving the market. Furthermore, investments are also provided by the government to support them. Thus, this promotes the market growth.
Asia-Pacific Emerges as the Fastest Lane for the Respiratory Revolution
The Asia-Pacific region became the fastest-growing region as a result of increased pollution, growing populations, and improved disease literacy. Within emerging economies, expanding healthcare infrastructure and governmental support have presented introduction opportunities for biologics, digital monitoring devices, and low-cost asthma medications.
China was leading the Asia-Pacific region in the asthma treatment market due to its rapid healthcare modernization, increased asthma research, and strong domestic pharmaceutical production. Further, government policies and regulations to support local drug manufacturing and advance digital inhaler development improved their affordability and accessibility across large cities.
Asia-Pacific Emerges as the Fastest Lane for the Respiratory Revolution
The Asia-Pacific region became the fastest-growing region as a result of increased pollution, growing populations, and improved disease literacy. Within emerging economies, expanding healthcare infrastructure and governmental support have presented introduction opportunities for biologics, digital monitoring devices, and low-cost asthma medications.
China was leading the Asia-Pacific region in the asthma treatment market due to its rapid healthcare modernization, increased asthma research, and strong domestic pharmaceutical production. Further, government policies and regulations to support local drug manufacturing and advance digital inhaler development improved their affordability and accessibility across large cities.
Europe - The Smart Medicine Frontier
Europe is expected to grow rapidly in the asthma treatment market due to advanced healthcare, strict environmental laws, and high use of biology. Increased government support for sustainable inhalers and advanced diagnostics provided many opportunities for innovation and precision therapies for asthma.
Germany led the European asthma treatment market with strong R&D facilities, as well as early use of biologics and insurance coverage. In addition, Germany's focus on digital health and eco-friendly inhalers (e.g., DPI instead of pMDI) enhanced its position as a leader in asthma treatment innovation.
Latin America – Emerging Strong: Fresh Air in the Pharma Scene
The steady growth of the LATAM market was due to a combination of increased asthma prevalence, access to healthcare, and awareness campaigns. Growing opportunities for global and domestic manufacturers were supported by the government's expansion of the pharmaceutical industry's capacity to respond to natural asthma treatments at an affordable cost.
Brazil had the largest number of patients, significant local pharmaceutical development, and an established national respiratory health program. The government's recognition of the need to allow for affordable, available inhalers helped solidify the country's overall capacity to treat asthma.
Middle East & Africa – The New Dawn for Respiratory Health
The Middle East & Africa region saw moderate growth in the asthma treatment market due to healthier funding levels, increased pollution, and rising incidence of asthma diagnosis. International collaboration with both the public and private sectors on health initiatives presents opportunities for registered drug products and smart inhaler adoption.
Saudi Arabia has had a strong commitment to investment in healthcare infrastructure in the form of new hospitals, and awareness programs for respiratory diseases. National programs encouraged tools and local medicine formulation using artificial intelligence to support the growth of new asthma medicines.
Asthma Treatment Market Companies
- AstraZeneca
- Teva Pharmaceutical Industries Ltd.
- GlaxoSmithKline plc
- Boehringer Ingelheim International GmbH
- Roche Holding AG / Novartis AG
- Merck & Co., Inc.
- Koninklijke Philips N.V.
- Sanofi-Aventis SA
- MundiPharma.
Recent Developments
- In April 2025, a collaboration, along with funding support and technical assistance from the PATH-CITED TA Market Place and the Department of Health Care Services PATH-CITED Grant Initiative, for the launch of an Asthma Remediation Community Supports (AR-CS) Initiative, was announced by Vivant Health and Community Resource Project, Inc. (CRP). To help the families and individuals in the greater Sacramento region, affected by asthma, will be the main goal of this initiative. (Surce: https://www.morningstar.com)
- In May 2025, the launch of a new Phase IIIb/IV clinical trial, for AIM4, was announced by the collaboration between Sanofi and Regeneron at the American Thoracic Society (ATS) 2025 Congress held on 19 May during the evening industry conference. Furthermore, in patients with uncontrolled medium-dose ICS/LABA, the evaluation of earlier biologic intervention with dupilumab would provide larger outcomes when compared with high-dose inhaled corticosteroids (ICS), in a stepwise manner to enhance the asthma care, which will be the main objective of this trial. (Source: https://www.pharmaceutical-technology.com)
Market Segmentation
By Medication
- Quick-relief medication
- Long-term control medication
By Route of Administration
- Inhalers
- Prefilled syringes/vials
- Others
By Adjunct Therapy
- LAMA (long-acting muscarinic antagonists)
- LABA (long-acting beta antagonists)
- Others
By Distribution Channel
- Online pharmacies
- Hospital pharmacies
- Retail pharmacies & drug stores
By Region
- North America
- Latin America
- Europe
- Asia-pacific
- Middle and East Africa
For inquiries regarding discounts, bulk purchases, or customization requests, please contact us at sales@precedenceresearch.com
Frequently Asked Questions
Ask For Sample
No cookie-cutter, only authentic analysis – take the 1st step to become a Precedence Research client
 Get a Sample
Get a Sample
 Table Of Content
Table Of Content
.webp)

 sales@precedenceresearch.com
sales@precedenceresearch.com
 +1 804-441-9344
+1 804-441-9344
 Schedule a Meeting
Schedule a Meeting
