This blog explains medical waste classification potential risks and treatment approaches. It highlights the importance of safe handling disposal methods and regulatory compliance to protect healthcare workers the environment and public health.
Medical waste refers to waste generated from healthcare activities, including physicians’ offices, dental practices, blood banks, veterinary clinics, and research facilities and laboratories. According to the World Health Organization (WHO), it includes materials that may be infectious, hazardous, or potentially harmful if not handled properly.
Despite its significance today, medical waste was not always subject to structured regulation. In the past, it was often discarded into the regular waste stream, increasing the risk to public health. The need for systematic waste management began to emerge in the mid-1800s, when Edwin Chadwick highlighted poor sanitary conditions in British hospitals and prisons, leading to the Public Health Act of 1848. This marked an early effort to improve public health standards, although consistent regulation evolved gradually over time.
Medical waste later became one of the last waste streams to be formally regulated in the United States. The Solid Waste Disposal Act of 1965 was introduced to reduce waste and protect human and environmental health, followed by the Resource Conservation and Recovery Act of 1976, which established a framework for managing hazardous and solid waste. Further regulatory control was introduced through the Medical Waste Tracking Act of 1988, under which the Environmental Protection Agency (EPA) implemented waste management regulations starting in 1989 across selected states.
In addition to the EPA, several federal agencies, including the CDC, FDA, DOT, and OSHA, have established safety guidelines governing the handling and disposal of medical waste. Today, with increasing healthcare activities and stricter regulatory oversight, proper handling, segregation, and containment of medical waste have become critical, reinforcing the role of specialized medical waste containers in ensuring compliance and safety.
What is the Medical Waste Containers Market Size in 2026?
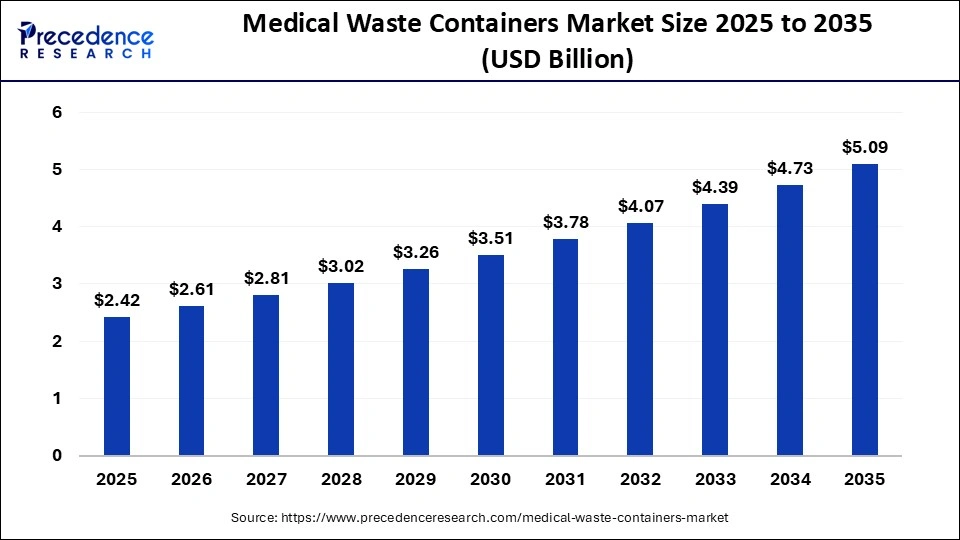
The global medical waste containers market size was valued at USD 2.42 billion in 2025 and is predicted to increase from USD 2.61 billion in 2026 to approximately USD 5.09 billion by 2035, expanding at a CAGR of 7.72% from 2026 to 2035. Rising healthcare expenditure and infrastructure development, coupled with increasing volumes of medical waste, are key factors driving growth in the market.
Get a Free Sample Report with Key Market Trends: https://www.precedenceresearch.com/sample/8220
Classification of Medical Waste
Medical waste is broadly classified into several categories based on its nature, risk level, and source of generation. Each type requires specific handling, segregation, and disposal practices to ensure safety and regulatory compliance.
- Chemical waste: This category includes waste generated from laboratory and medical processes involving chemicals such as solvents, reagents, disinfectants, and sterilants. It also covers heavy metals found in medical devices, such as mercury in broken thermometers, as well as batteries.
- Infectious waste: Infectious waste refers to materials that are known or suspected to contain pathogens and that pose a risk of disease transmission. This includes waste contaminated with blood and other body fluids, laboratory cultures, microbiological stocks, and materials that have been in contact with patients suffering from highly infectious diseases.
- Non-hazardous or general waste: This type of waste does not pose any specific biological, chemical, radioactive, or physical hazard. It typically includes general healthcare waste that is not contaminated or otherwise harmful in nature.
- Pathological waste: Pathological waste consists of human tissues or body parts and bodily fluids, along with fetuses, unused blood products, and contaminated animal carcasses generated from medical or research activities.
- Pharmaceutical and cytotoxic waste: This category includes expired, unused, or contaminated pharmaceutical products. Cytotoxic waste specifically refers to substances with genotoxic properties, such as cytostatic drugs used in cancer treatment, as well as related contaminated materials.
- Radioactive waste: Radioactive waste comprises materials contaminated with radionuclides, including waste generated from diagnostic or radiotherapeutic procedures in healthcare settings.
- Sharps waste: Sharps waste includes items capable of causing cuts or puncture injuries, such as needles, syringes with attached needles, infusion sets, scalpels, pipettes, knives, blades, and broken glass.
Hazards Associated with Medical Waste
Medical waste presents a range of health, environmental, and occupational hazards, particularly when it is not properly handled, segregated, or disposed of. These risks vary depending on the type of waste and the level and duration of exposure.
- Infectious and disease-related hazards: Medical waste can contribute to the spread of lung infections, parasitic infections, skin infections, and gastrointestinal infections. It is also associated with the transmission of serious viral diseases such as HIV, hepatitis B, and hepatitis C, with reported transmission risks of approximately 0.3%, 3%, and 5%, respectively, from infected waste. Additional risks include bacterial infections, septicemia, candidemia, cholera, tuberculosis, AIDS, ocular infections, respiratory infections, and other conditions caused by exposure to contaminated materials.
- Occupational and injury-related hazards: Handling medical waste poses significant occupational risks, particularly due to sharps, which remain a major source of injuries such as needlestick incidents. These injuries often go unnoticed among informal waste handlers, such as rag pickers, increasing their vulnerability to infection and related complications. Occupational risks are further highlighted by WHO estimates, which indicate that around 54% of healthcare workers in low- and middle-income countries have latent tuberculosis, significantly higher than in the general population.
- Radioactive hazards: Exposure to radioactive medical waste, including materials contaminated with radionuclides such as iodine-131, can lead to adverse health effects depending on the intensity and duration of exposure. Radioactive solid waste often includes contaminated syringes, needles, cotton, swabs, gauze, gloves, and absorbent materials, along with waste generated from patients undergoing high-dose treatments. Symptoms may range from dizziness, nausea, and headaches to severe outcomes such as tissue damage and cellular destruction.
- Chemical hazards: Exposure to chemical waste can lead to poisoning as a result of direct contact or inhalation. Both short-term and long-term exposure can result in intoxication, while physical injuries such as chemical burns are also commonly observed.
- Pharmaceutical and genotoxic hazards: Improper disposal of pharmaceuticals can lead to their entry into the ecosystem, often through sewage systems, resulting in contamination of groundwater, surface water, and soil. Cytotoxic and other genotoxic compounds, including those used in cancer therapy, pose additional risks due to their harmful effects on biological systems.
- Environmental hazards: Improper segregation and disposal of biomedical waste can contaminate groundwater and contribute to the spread of infection among humans and animals, from hospital waste storage areas to landfills. Inadequate containment increases risks from birds, rodents, and stray animals. Additionally, improper containment, aggregation, and incineration can release airborne pollutants, which may spread over inhabited areas and trigger multiple health issues.
- Regulatory and system-related risks: Improper containment, segregation, and incineration, both on-site and off-site, can lead to inefficiencies in the waste management system and failure to meet regulatory standards, increasing the likelihood of environmental contamination and associated health risks.
Waste-Specific Treatment pathway
- Infectious waste: This category is primarily treated using low-heat thermal processes such as autoclaving and microwaving, where controlled heat and moisture are used to eliminate microbial contamination before further processing or disposal.
- Pathological waste: This type of waste is directed towards high-temperature treatment methods, mainly incineration, to ensure destruction and safe reduction of organic matter.
- Chemical waste: Chemical waste requires controlled treatment depending on its composition. Certain categories undergo chemical neutralization or high-temperature processing under regulated conditions to prevent environmental release.
- Pharmaceutical and cytotoxic waste: This category is treated through high-temperature incineration to break down complex chemical compounds and ensure that harmful residues are not released into the environment.
- Radioactive waste: Instead of immediate processing, this waste is managed through controlled storage until its radioactivity reduces to a permissible level, followed by regulated disposal.
- Non-hazardous (general) waste: This waste is typically managed through mechanical processes such as compaction and shredding to reduce volume and ensure safe disposal.
- Sharps waste: Sharps waste is first disinfected using methods like autoclaving or chemical treatment, followed by shredding or destruction to eliminate the risk of reuse and injury.
- Organic waste: Organic components are treated using biological processes involving enzymes, which help reduce the biological load before final disposal.
| Green Dustbin | Blue Dustbin | Red Dustbin | Yellow Dustbin | Black/Grey Dustbin |
| Biodegradable and organic waste (food, garden waste) | Dry waste and recyclable items (plastic, glass, paper, metals) | Hazardous or biomedical waste | Sanitary and medical waste | General waste not suitable for recycling |
Note: The color code sometimes depends on regional regulatory practices.
Global Adoption of Medical Waste Containers
North America contributes to the highest adoption of medical waste containers, propelled by advanced waste management technologies and stringent regulations like the Resource Conservation and Recovery Act (RCRA). Key authorities, including DOT, OSHA, EPA, and state regulators, mandate that healthcare facilities utilize certified containers, ensuring safety and compliance. The U.S. leads revenue contributions, driven by investment in sustainable solutions and large healthcare systems generating substantial waste.
In contrast, Asia-Pacific is expected to grow fastest due to industrialization, expanding healthcare, and government regulations that increase waste volumes. China’s market is fueled by new healthcare facilities and enhanced environmental awareness. Innovations such as converting saline containers into fuel and tools like Cortech’s SafeBin are improving waste disposal safety. In India, despite regulatory frameworks, challenges persist in compliance and technology adoption. Solutions like AI sensor containers and automated systems aim to enhance waste management efficiency as healthcare evolves.
Expert Advise
According to our analysis, medical waste containers are essential components in the healthcare ecosystem to comply with stringent regulations. Medical waste containers are frontline defense systems in infection control, occupational safety, and environmental protection. Stakeholders focus on multiple aspects, such as standardization, material quality and design, and behavioral reinforcement, enabling developers to produce customized containers based on the needs. The future of medical waste containers is promising, driven by smart and sustainable innovation and the shift toward eco-friendly materials.
About the Authors

Aditi Shivarkar
Aditi, Vice President at Precedence Research, brings over 15 years of expertise at the intersection of technology, innovation, and strategic market intelligence. A visionary leader, she excels in transforming complex data into actionable insights that empower businesses to thrive in dynamic markets. Her leadership combines analytical precision with forward-thinking strategy, driving measurable growth, competitive advantage, and lasting impact across industries.

Aman Singh
Aman Singh with over 13 years of progressive expertise at the intersection of technology, innovation, and strategic market intelligence, Aman Singh stands as a leading authority in global research and consulting. Renowned for his ability to decode complex technological transformations, he provides forward-looking insights that drive strategic decision-making. At Precedence Research, Aman leads a global team of analysts, fostering a culture of research excellence, analytical precision, and visionary thinking.

Piyush Pawar
Piyush Pawar brings over a decade of experience as Senior Manager, Sales & Business Growth, acting as the essential liaison between clients and our research authors. He translates sophisticated insights into practical strategies, ensuring client objectives are met with precision. Piyush’s expertise in market dynamics, relationship management, and strategic execution enables organizations to leverage intelligence effectively, achieving operational excellence, innovation, and sustained growth.





 Request Consultation
Request Consultation

