A detailed look at the evolving role of back end revenue cycle management in healthcare systems. It covers challenges such as claim denials data fragmentation and compliance while emphasizing AI driven solutions for better revenue capture and financial stability.
Healthcare systems worldwide are facing mounting financial pressure driven by rising operational costs and reimbursement complexities. Clinical innovation is still rapidly evolving, but financial systems are unable to keep up with changing payer needs and regulatory expectations. In this difficult setup, back-end revenue cycle management is the most essential and underrecognized functioning field.
Back-end processes constitute the last gateway through which healthcare services are translated into the achieved financial results. These are claims validation processes, code accuracy processes, denial processes, and payment reconciliation processes. Inefficiency in these processes directly affects the stability of the cash flow and the long-term sustainability of the organization.
Current trends in operations within big hospital networks show that healthcare executives are becoming more aware. The quality of financial performance is no longer based on the patient volume or the quality of services alone, but on the efficiency of revenue capture systems. Furthermore, back-end revenue cycle management is shifting away from an administrative requirement to a strategic focus of healthcare management.
A System Under Pressure: Why Back-End Complexity is Increasing Rapidly
The nature of changing healthcare ecosystems and payer dynamics has contributed to making the concept of back-end revenue cycle management better and more complex. The present-day healthcare organizations have to manoeuvre their way through a disjointed environment of insurance companies and other payment systems. Different payers have their own set of rules, documentation, and reimbursement patterns that make the work of claims processing complex.
Latest trends in payer behavior refer to the harder implementation of coding accuracy and documentation requirements. The allegations that checks that are once known to have been approved by the validation can be re-evaluated and rejected on grounds of minor discrepancies or omissions of information. The mentioned stricting of needs is compelling healthcare organizations to embrace stricter validation measures in back-end processes.
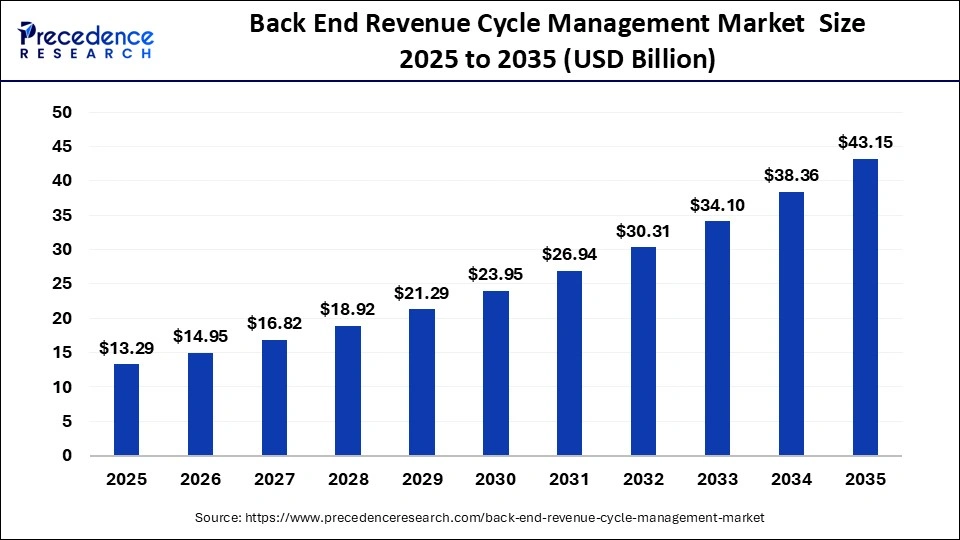
What is the Back End Revenue Cycle Management Market Size in 2026?
The global back end revenue cycle management market was valued at USD 13.29 billion in 2025 and is projected to grow from USD 14.95 billion in 2026 to approximately USD 43.15 billion by 2035, registering a CAGR of 12.50% from 2026 to 2035. This growth is driven by rising claim denials, increasing reimbursement complexity, and the growing adoption of automation in back-end revenue cycle operations.
Get a Free Sample Report with Key Market Trends: https://www.precedenceresearch.com/sample/8215
Where Revenue Actually Breaks: Understanding the Denial Economy
The increasing rate of claim denials is one of the biggest issues in back-end revenue cycle management. Denials are late payments and lost opportunities that have to be further worked on by the administrator. Denial management is now a functional operation in most healthcare systems, with special teams and processes.
Core Back-End Functions Under Transformation
| Operational Area | Transformation Focus in Modern Systems |
| Claims Processing | Automation of submission workflows and validation checks |
| Denial Management | Predictive analytics to identify and prevent claim rejections |
| Payment Posting | Real-time reconciliation of payments and adjustments |
| Coding Accuracy | AI-assisted coding validation and compliance monitoring |
| Payer Communication | Digital platforms for faster dispute resolution and coordination |
The latest analytics integrations in the healthcare system are disclosing new details about the trends in denials. Machine learning models are detecting similar trends that point to system-wide problems in documentation or codes of practice. Such understandings are helping organizations to stop responding to denials reactively and start intercepting the denials proactively.
Rewriting the Workflow: From Linear Processing to Intelligent Pipelines
Traditional back-end revenue cycle workflows follow a linear structure where tasks are executed sequentially from claims submission to payment reconciliation. The method tends to cause bottlenecks in situations where problems arise at any point in the process. Any delays in a single step may have a trickle effect on the entire workflow and affect overall efficiency.
Linear workflows are being substituted with intelligent processing pipelines, which are very dynamic and run simultaneously. These pipelines take advantage of automation and analytics to detect and fix problems immediately.
These intelligent pipelines are taking on real-time validation engines. These systems compare the payer requirements and coding standards with the previous patterns of data and analyze claims. Early detection of discrepancies can help organizations achieve high levels of reduction in rejection rates and also enhance efficiency in the processing.
Automation at Scale: Eliminating Friction Without Losing Control
Automation is slightly undergoing a transformative role in the redesign of back-end revenue cycle functions in healthcare systems. Monotonous duties, including claim entry, payment recording, and reconciliation, are becoming the responsibility of robotic process automation systems. These systems are able to execute the workflow with precision and consistency, minimizing human error and processing delays.
Automation is not simply about replacing manual tasks with software-driven processes. It must be planned meticulously so that the process involved can be transparent and easily manageable. Companies need to adopt a monitoring mechanism that brings about visibility of the automated processes and allows intervention when there is a need to do so.
Artificial Intelligence is Introducing Predictive Financial Control
Artificial intelligence (AI) can add the element of prediction, which transforms financial control in health care systems. AI is used to process data on claims in the past, payer relationships, and operational trends to predict the occurrence of a risk before it occurs. This is because overcoming this barrier will enable organizations to act proactively as opposed to responding to challenges once they arise.
Natural language processing technologies are also enhancing documentation accuracy by extracting relevant information from clinical notes. These systems are very helpful in keeping the billing codes consistent with the documented care, minimizing the discrepancies, and enhancing compliance. In the coming years, such AI-based capabilities will result in a feedback mechanism that is constantly enhancing financial performance.
The Rise of Revenue Intelligence Platforms
There is growing use of an integrated revenue intelligence platform in healthcare organizations. The platforms will give real-time visibility on the claims, denial patterns, and payment cycles within the organization. Such a degree of transparency allows leaders to make effective decisions within a short period of time.
Another important aspect of these platforms is the ability to simulate financial situations depending on the alterations in the operation. Organizations are able to determine the possible influences of policy changes, coding, or improvement of processes before they can be implemented. This is a capability to help in strategic planning, and uncertainty in decision-making is minimized.
Operational Models are Evolving Beyond Traditional Boundaries
The transformation of back-end revenue cycle management is driving changes in how healthcare organizations structure their operations. Various systems are centrally concentrating financial functions in specific revenue cycle hubs, which are serving more than one facility. This solution enhances coordination and uniformity of workflows.
Outsourcing is also emerging as a strategic choice to deal with complicated back-end operations. The specialized service providers specialize in fields like denial management, coding validation, and compliance monitoring. Through the option of outsourcing, an organization can improve performance without the need to make huge investments internally.
Blended models of internal and external partners are becoming more popular as a middle ground. The latter models enable companies to maintain control over major functional areas and achieve the advantages of expertise. This flexibility comes in especially when dealing with dynamic healthcare settings.
Compliance as a Continuous Discipline, Not a Periodic Task
Regulatory compliance is one of the key issues in back-end revenue cycle management that has to be addressed and changed constantly. Healthcare organizations are to comply with the changing standards of the billing practices, coding specifications, and patient information security. Failure to comply may lead to fines, audit inspection, and loss of reputation.
Current regulatory trends are making compliance requirements more complex, especially within value-based care setups. Efforts by providers to show the relationship between clinical outcome and reimbursement structure will introduce new dimensions to the financial operations. This change highlights the need to incorporate compliance in all the phases of the revenue cycle.
Data Fragmentation is Being Replaced by Unified Financial Visibility
The problem of data fragmentation has always been a setback to efficient back-end revenue cycle management in healthcare systems. Claims, payments, and clinical documentation information are often stored in separate systems, making it hard to see. Such failure to be integrated results in blind spots, which lead to hindrance of optimization of decisions and performance.
The use of advanced analytics tools is also driving the use of data further by generating predictive information based on historical data. The insights allow organizations to predict the changes in revenue, streamline workflows, and allocate resources. This is causing data to become a strategic asset that leads to continuous improvement.
Persistent Barriers That Continue to Shape Adoption
Despite significant advancements, several challenges continue to influence the adoption of modern back-end RCM systems. The continued existence of legacy infrastructure is also a significant challenge, as a high number of organizations are running outdated systems that are hard to integrate. Renovation of these systems involves a lot of planning and high investment.
The issues of cybersecurity are gaining prominence as financial systems become more computerized. Protecting sensitive patient and financial data requires robust security frameworks and continuous monitoring. Innovation has to be weighed against security in organizations to preserve trust and compliance.
Toward Autonomous Revenue Cycle Ecosystems
The future of back-end revenue cycle management is leaning towards autonomous ecosystems with the development of AI. These systems keep track of workflow processes, learn and apply corrective measures without the need for manpower. This development is a great leap forward compared to present-day operational models.
Integration with clinical systems will further enhance accuracy by aligning billing processes with patient care activities. This minimizes discrepancies and enhances adherence to reimbursement requirements. Furthermore, with the maturity of such systems, healthcare organizations will gain the financial accuracy that has never been witnessed before.
Conclusion: Financial Mastery Will Define Healthcare Leadership
Back-end revenue cycle management ceases to be a peripheral activity in contemporary healthcare institutions. It has become a defining factor that influences financial stability, operational efficiency, and long-term growth. Those organizations that invest in the modernization of these systems are placing themselves in a position of success in an ever-more complex environment.
Since the healthcare systems are undergoing continuous changes, back-end RCM becomes even more central to the organizational outcomes. The future of financial operations will be characterized by precision, smartness, and flexibility. Those who successfully embrace this transformation will lead the industry in both performance and resilience.
Expert Advise
Our experts suggest that back end revenue cycle management has become a financial control center for healthcare organizations. Rising denial complexity, workforce pressure, and fragmented systems encourage healthcare organizations to adopt advanced RCM solutions. The integration of AI and ML into RCM solutions introduces automation, resulting in faster reimbursements and fewer errors. The future is driven by AI bots to handle end-to-end claims lifecycle. Back-end RCM tools address the complexities of the disrupted claims approval processes, enhancing treatment accessibility and affordability.
About the Authors

Aditi Shivarkar
Aditi, Vice President at Precedence Research, brings over 15 years of expertise at the intersection of technology, innovation, and strategic market intelligence. A visionary leader, she excels in transforming complex data into actionable insights that empower businesses to thrive in dynamic markets. Her leadership combines analytical precision with forward-thinking strategy, driving measurable growth, competitive advantage, and lasting impact across industries.

Aman Singh
Aman Singh with over 13 years of progressive expertise at the intersection of technology, innovation, and strategic market intelligence, Aman Singh stands as a leading authority in global research and consulting. Renowned for his ability to decode complex technological transformations, he provides forward-looking insights that drive strategic decision-making. At Precedence Research, Aman leads a global team of analysts, fostering a culture of research excellence, analytical precision, and visionary thinking.

Piyush Pawar
Piyush Pawar brings over a decade of experience as Senior Manager, Sales & Business Growth, acting as the essential liaison between clients and our research authors. He translates sophisticated insights into practical strategies, ensuring client objectives are met with precision. Piyush’s expertise in market dynamics, relationship management, and strategic execution enables organizations to leverage intelligence effectively, achieving operational excellence, innovation, and sustained growth.





 Request Consultation
Request Consultation

