What is the Back End Revenue Cycle Management Market Size in 2026?
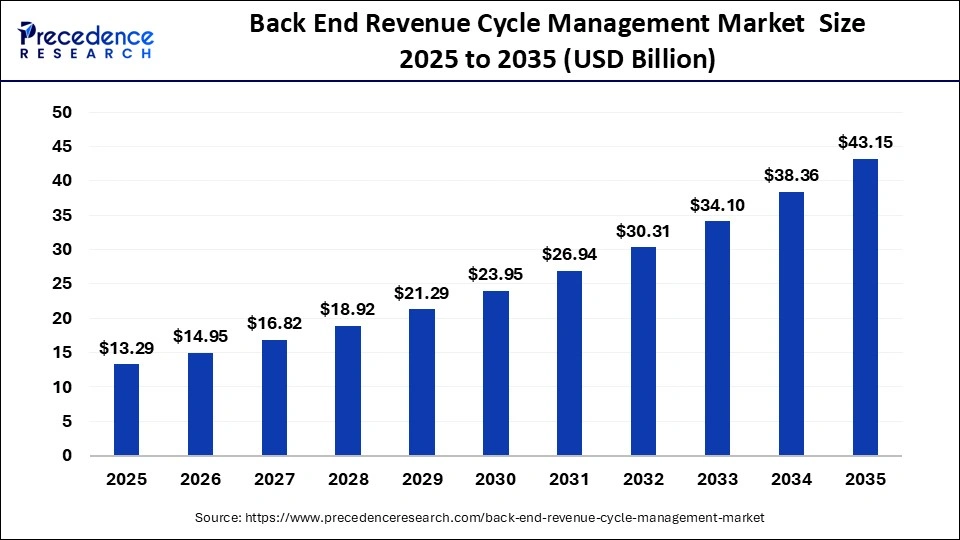
The global back end revenue cycle management market size was calculated at USD 13.29 billion in 2025 and is predicted to increase from USD 14.95 billion in 2026 to approximately USD 43.15 billion by 2035, expanding at a CAGR of 12.50% from 2026 to 2035. The market growth is attributed to rising claim denials, increasing reimbursement complexity, and growing adoption of automation in back-end revenue cycle operations.
Key Takeaways
- North America dominated the market with a share of 46.8% in 2025.
- Asia-Pacific is expected to grow at the fastest CAGR between 2026 and 2035.
- By function, the claims submission segment contributed the highest back end revenue cycle management market share of 21.8% in 2025.
- By function, the denial management segment is expected to grow at a strong CAGR of 12.8% between 2026 and 2035.
- By component, the services segment held a major market share of 57.4% in 2025.
- By component, the software segment is expected to expand at the fastest CAGR of 12.4% from 2026 to 2035.
- By deployment mode, the cloud-based segment held the largest market share of 51.8% in 2025 and is expected to expand rapidly in the market with a CAGR of 14.1% in the coming years.
- By end user, the hospitals segment generated the biggest market share of 48.6% in 2025.
- By end user, the ambulatory surgical centers segment is expected to grow at the highest CAGR of 12.7% between 2026 and 2035.
Which Factors Drive the Back End Revenue Cycle Management Market?
Rising claim denials and growing reimbursement complexity are strongly driving the global back end revenue cycle management (RCM) industry. Medical professionals are also gradually moving towards organized mechanisms of collecting payment and cutting down on revenue loss. Back-end RCM technology comprises medical coding, claims submission, denial management, payment posting, and accounts receivable.
These systems provide accurate payer reimbursement and enhance financial control. The American Hospital Association stated that RCM AI tools decreased claim dismissals by up to 22% in 2024. Furthermore, as healthcare systems shift toward value-based care, payer structures are becoming more complex. This further increases dependence on efficient back-end RCM solutions, reinforcing market growth as a key driver.
Back End Revenue Cycle Management Market Growth Factors
- Rising Complexity of Multi-Payer Healthcare Systems: Increasing variations in payer policies are fuelling the need for advanced back-end RCM platforms.
- Growing Demand for Financial Transparency in Healthcare: Enhanced focus on revenue visibility is propelling adoption of analytics-driven back-end RCM technologies.
Driving Forces and Pressures Reshaping the Back End Revenue Cycle Management Market
- According to the Centers for Medicare & Medicaid Services, Medicare and Medicaid accounted for 7.8% and 6.6% of total U.S. healthcare spending, respectively, in 2024, increasing complexity in back-end RCM workflows.
- According to the American Medical Association, up to 12% of medical claims were submitted with inaccurate codes in 2024, increasing back-end RCM rework and denial management burden.
- According to Healthcare Financial Management Association survey data, 44% of healthcare organizations outsourced part or all of RCM functions in 2024, accelerating global back-end RCM outsourcing adoption.
- According to the Healthcare Financial Management Association, billing and collection costs accounted for approximately 3%–5% of total hospital revenue in 2024, emphasizing cost pressures within back-end RCM operations.
- According to the Centers for Medicare & Medicaid Services, improper payment rates in U.S. healthcare programs remained around 7%–8% in 2024, intensifying the need for fraud detection in back-end RCM systems.
Impact of Artificial Intelligence on the Back End Revenue Cycle Management Market
Artificial intelligence (AI) is significantly reshaping the market by enhancing efficiency, accuracy, and financial performance across healthcare organizations. The tools powered by AI are able to scan large amounts of claims and billing records to identify errors and forecast denials, and optimize coding mechanisms in real-time. Such capabilities ease the administrative burden and speed up the reimbursement processes to enhance revenue realization. Organizations are enforcing AI to automate most repetitive processes and to increase the scalability of operations.
Back End Revenue Cycle Management Market Trends
- Autonomous Revenue Cycle Platforms Reshaping Operational Models:Healthcare providers are progressively embracing independent systems in which claims, coding, and collections are handled with little human engagement. This change is making operations less complex and more scalable across wide healthcare systems and networks. There is a growing need for advanced solutions in back-end revenue cycle management among healthcare organizations in the world.
- Predictive Revenue Intelligence Driving Proactive Financial Management:The trend is to shift to predictive systems where organizations can detect revenue risks prior to the payment being sent to payers. These tools can help providers avoid mistakes at the initial stage and enhance accuracy to minimize reliance on manual corrections. This development is reinforcing the position of analytics-based back-end RCM systems in improving the bottom line.
Market Scope
| Report Coverage | Details |
| Market Size in 2025 | USD 13.29 Billion |
| Market Size in 2026 | USD 14.95 Billion |
| Market Size by 2035 | USD 43.15 Billion |
| Market Growth Rate from 2026 to 2035 | CAGR of 12.50% |
| Dominating Region | North America |
| Fastest Growing Region | Asia-Pacific |
| Base Year | 2025 |
| Forecast Period | 2026 to 2035 |
| Segments Covered | Function, Component, Deployment Mode, End User, and Region |
| Regions Covered | North America, Europe, Asia-Pacific, Latin America, and Middle East & Africa |
Back End Revenue Cycle Management Market Market Dynamics
Driver
Increasing Complexity of Multi-Payer Reimbursement Structures
Increasing variation in payer policies and reimbursement rules is expected to intensify demand for structured back-end revenue cycle systems. Organizations are also emphasizing high-performance systems that standardize interactions with payers and enhance claim accuracy in various reimbursement models. Furthermore, such dynamics are strengthening the role of back-end revenue cycle platforms in managing payer-driven operational complexity.
Restraint
High Implementation and Integration Costs
High upfront investment requirements are expected to hamper the market growth across small and mid-sized providers. Healthcare organizations incur hefty expenses in terms of software implementation, customization of the system, and infrastructure upgrades. Moreover, the impending shortage of trained professionals in medical coding, billing, and analytics is projected to affect the efficiency of back-end revenue cycle operations.
Opportunity
Spurring Adoption of Automation and AI in RCM
Spurring integration of AI and automation technologies is estimated to enhance efficiency across revenue cycle workflows, creating immense opportunities for the players competing in the market. The encouragement of AI and automation technology increases efficiency among various revenue cycle activities.
Reports indicate that 67% of healthcare organizations are already using AI in RCM processes as of 2026. Furthermore, companies are using technologies to enhance the efficiency of operations and financial performance. This technological shift is significantly driving the modernization of back-end revenue cycle management systems globally.
Segmental Insights
Function Insights
Which Function Segment Dominated the Back End Revenue Cycle Management Market?
The claims submission segment dominated the market in 2025, accounting for an estimated 21.8% market share, due to the rising volume of healthcare transactions and increasing reliance on electronic claim workflows across providers.Health systems receive billions of claims in a year, which generates high demand for correct and efficient submission systems. Furthermore, the constant urge to move to digital healthcare infrastructure has also pushed the acceptance of advanced claim submission technologies.
Back End Revenue Cycle Management Market Share, By Function, 2025-2035 (%)
| Function | 2025 | 2035 |
| Medical Coding | 14.60% | 12.80% |
| Charge Capture | 9.70% | 8.70% |
| Claims Submission | 21.80% | 19.70% |
| Payment Posting | 12.60% | 10.60% |
| Denial Management | 16.40% | 21.70% |
| Accounts Receivable Follow-Up | 13.80% | 12.70% |
| Revenue Integrity and Audit | 7.60% | 9.60% |
| Contract Management | 3.50% | 4.20% |
The denial management segment is expected to grow at the fastest CAGR of 12.8% in the coming years, owing to the rising levels of claims rejection and the financial strain on healthcare providers. Organizations are working towards establishing the root causes of denials to enhance the rate of recovery of revenue. The necessity to have better revenue retention and operational efficiency has prompted healthcare providers to build better capacities in denial management.
Component Insights
Back End Revenue Cycle Management Market Share, By Component, 2025-2035 (%)
| Component | 2025 | 2035 |
| Software | 42.60% | 48.70% |
| Services | 57.40% | 51.30% |
Why Did the Services Segment Dominate the Back End Revenue Cycle Management Market?
The services segment held the largest revenue share of 57.4% in the market in 2025, due to the increasing reliance on outsourcing for complex billing and collection processes. Medical professionals are giving attention to outside know-how to handle the accuracy of codes and payment documentation effectively. The necessity to control expenses and streamline processes is increasing the number of partnerships between healthcare organizations and third-party providers.
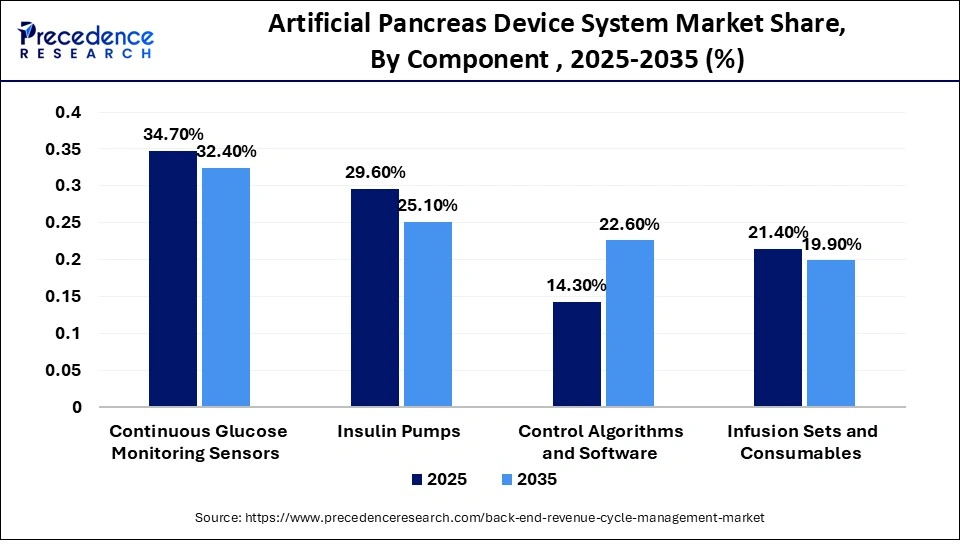
The software segment is expected to grow with the highest CAGR of 12.4% in the market during the studied years, owing to the rapid adoption of digital platforms and automation technologies. Medical institutions are moving to integrated systems that help simplify coding, billing, and denial management processes. Further software solutions are enhancing accuracy with real-time validation and decision-making using analytics. The move toward software-centric models is further increasing with the growing digital transformation initiatives.
Deployment Mode Insights
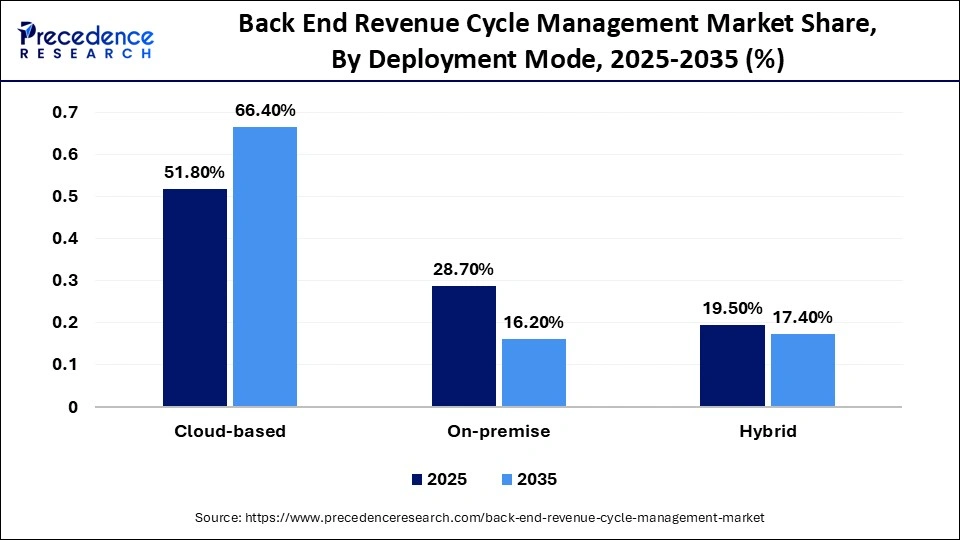
Back End Revenue Cycle Management Market Share, By Deployment Mode, 2025-2035 (%)
| Deployment Mode | 2025 | 2035 |
| Cloud-based | 51.80% | 66.40% |
| On-premise | 28.70% | 16.20% |
| Hybrid | 19.50% | 17.40% |
How the Cloud-Based Segment Dominated the Back End Revenue Cycle Management Market?
The cloud-based segment dominated the market in 2025, accounting for an estimated 51.8% market share and is expected to show the fastest growth with a CAGR of 14.1% over the forecast period, due to the increasing shift toward scalable and centralized digital infrastructure across healthcare organizations. Providers have been focusing on scalable systems that are used over the internet and on multi-location operations without having to invest heavily in capital expenditure.
Cloud platforms support real-time data synchronization and enhance billing accuracy, and hasten the reimbursement cycle. Healthcare providers are investing in smart cloud solutions that support predictive analytics and real-time performance monitoring. According to the Healthcare Information and Management Systems Society, over 70% of healthcare organizations adopted cloud-based IT solutions by 2025. Furthermore, the trend is making cloud deployment a rapidly growing area of back-end revenue cycle management.
End User Insights
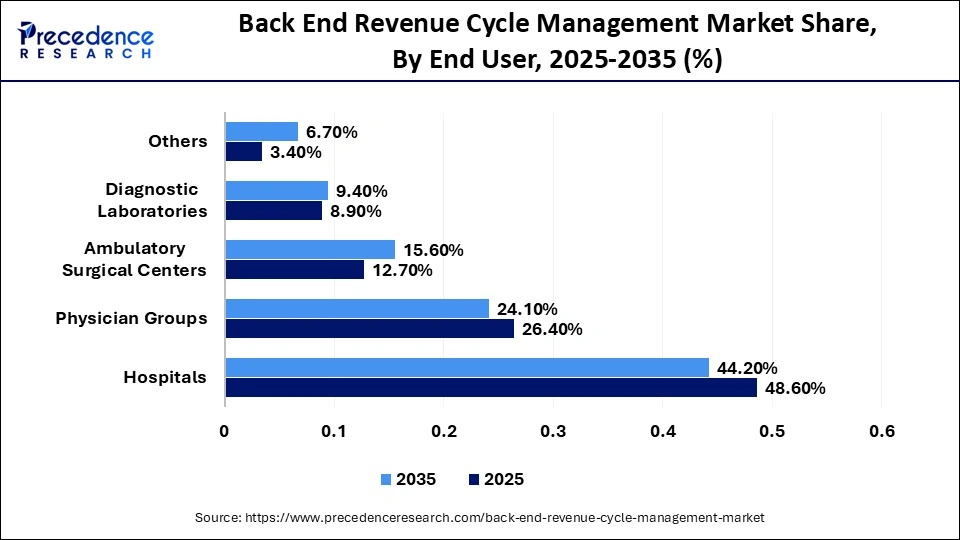
Back End Revenue Cycle Management Market Share, By End User, 2025-2035 (%)
| End User | 2025 | 2035 |
| Hospitals | 48.60% | 44.20% |
| Physician Groups | 26.40% | 24.10% |
| Ambulatory Surgical Centers | 12.70% | 15.60% |
| Diagnostic Laboratories | 8.90% | 9.40% |
| Others | 3.40% | 6.70% |
Which End User Segment Led the Back End Revenue Cycle Management Market?
The hospitals segment led the market with a share of 48.6% in 2025, due to the high volume of inpatient and outpatient services requiring complex billing workflows. Hospitals handle extensive clinical documentation, which requires accurate coding and detailed claim submission systems. The offerings of multi-specialty services also make matters even more complicated, making it a necessary approach to the use of high-level RCM systems. The developments are strengthening the leadership of hospitals throughout the end-user landscape in the market.
The ambulatory surgical centers segment is expected to witness the fastest growth in the market with a CAGR of 12.7% over the forecast period, owing to the increased tendency to adopt outpatient care provision models. Medical institutions are also moving their operations to less expensive outpatient facilities instead of the ever-traditional hospitals. These trends are increasing the demand for efficient revenue cycle systems fitted in the high-volume ambulatory surgical centers.
Regional Insights
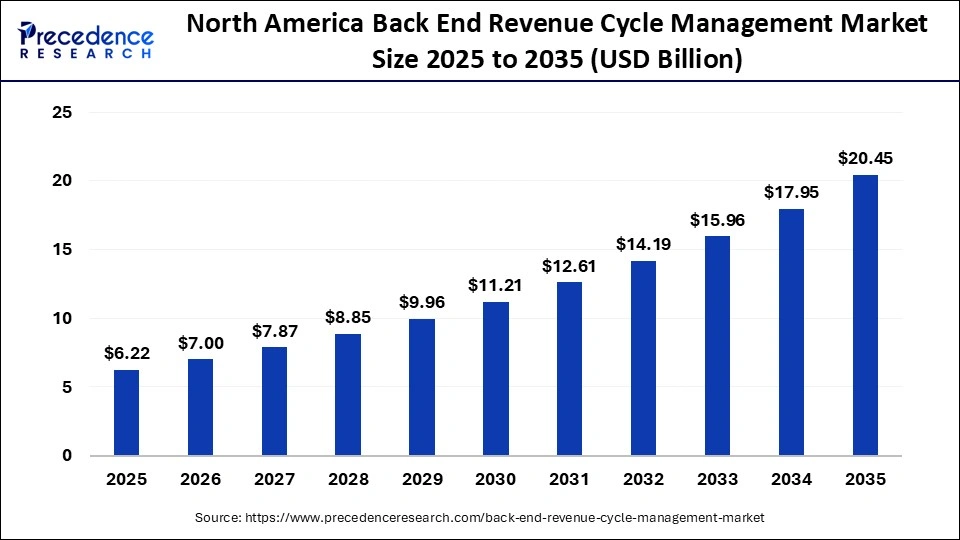
North America Back End Revenue Cycle Management Market Size and Growth 2026 to 2035
The North America back end revenue cycle management market size is estimated at USD 6.22 billion in 2025 and is projected to reach approximately USD 20.45 billion by 2035, with a 12.64% CAGR from 2026 to 2035.
Why North America Dominated the Back End Revenue Cycle Management Market?
North America held a major market share of 46.8% in 2025, due to the highly advanced healthcare infrastructure and early adoption of digital financial systems. The area handles a huge amount of insurance claims, and it creates more dependence on well-organized revenue cycle processes.
The high presence of major healthcare IT suppliers is enhancing the implementation of innovative RCM systems in hospitals and health organizations. According to the Centers for Medicare & Medicaid Services, healthcare spending in the U.S. grew 7.8% to USD 1,118 billion in 2024, which proves the ongoing investment in administrative technologies. Moreover, the growing focus of the providers is on reducing administrative costs and revenue leakage by using advanced solutions, which is further fuelling the regional growth in the market.
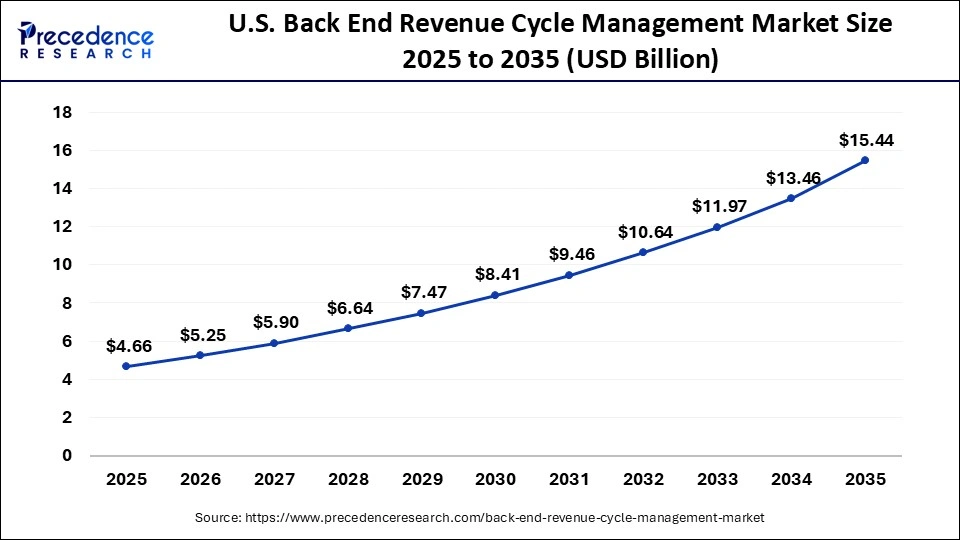
U.S. Back End Revenue Cycle Management Market Size and Growth 2026 to 2035
The U.S. back end revenue cycle management market size is calculated at USD 4.66 billion in 2025 and is expected to reach nearly USD 15.44 billion in 2035, accelerating at a strong CAGR of 12.73% between 2026 and 2035.
U.S. Driving Core Growth Engine in North America's Market
The U.S. leads the market in North America, driven by its highly complex multi-payer healthcare system and large claim processing volumes. Compliance and interoperability regulatory requirements are also driving providers towards digital solutions. These are boosting the existing dominance of the country in the adoption of back-end revenue cycle management.
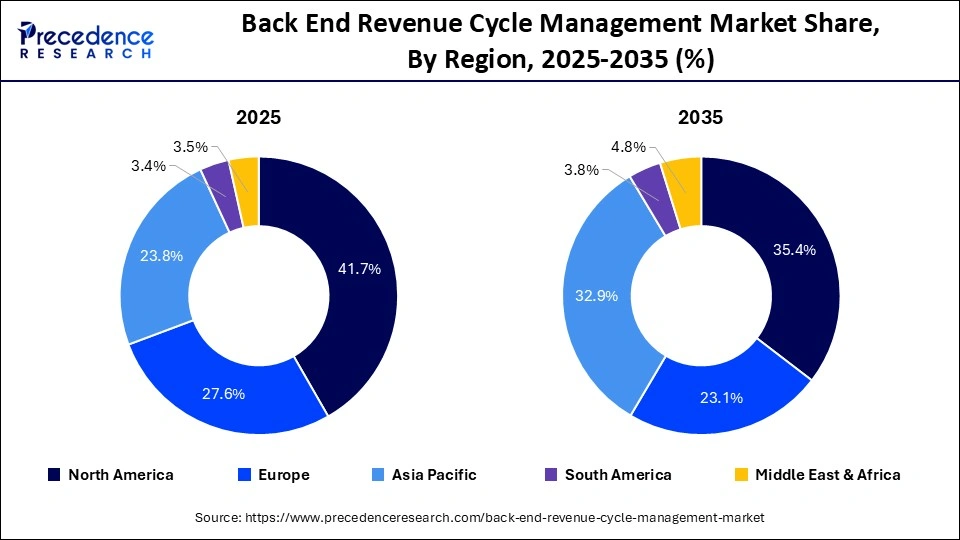
How is Asia Pacific Growing in the Back End Revenue Cycle Management Market?
Asia-Pacific is expected to experience the fastest growth during the predicted timeframe, owing to the growing healthcare facilities and the level of use of digital health technologies . The high rate of patient volumes is placing a higher burden on the need for an effective billing and reimbursement system. Furthermore, the growing need to conduct healthcare activities cost effectively is making Asia Pacific the fastest growing regional market in back-end revenue cycle management.
India: Emerging as a High Growth Country in Asia Pacific Market
India is leading the charge in the Asia Pacific market, as a result of the rapid healthcare digitalization and the increased growth of the private healthcare industry. The growth of hospital networks and diagnostic centers is also putting more pressure on scheduled revenue cycle operations. Moreover, these trends are increasing the uptake of back-end revenue cycle management solutions in the country.
Back End Revenue Cycle Management Market Value Chain Analysis

Back End Revenue Cycle Management Market Companies
- R1 RCM
- Optum
- Change Healthcare
- Conifer Health Solutions
- Cerner Corporation
- Epic Systems
- Athenahealth
- eClinicalWorks
- NextGen Healthcare
- Allscripts Healthcare Solutions
- Experian Health
- Waystar
- McKesson Corporation
- GE HealthCare
- AGS Health
Recent Developments
- In January 2026, Veradigm introduced an AI-enabled application for its Revenue Cycle Services clients to enhance financial insights and performance tracking. The solution targets challenges such as claim denials, staffing constraints, and limited revenue visibility in independent practices. This advancement emphasizes the increasing role of AI in optimizing revenue cycle efficiency and cash flow management. (Source: https://investor.veradigm.com )
- In June 2025, FinThrive launched FinThrive Fusion, a dynamic intelligence platform built on a modern data fabric for revenue cycle innovation. The platform delivers interoperability, automation, and scalable AI to address fragmentation in traditional RCM systems. This development highlights the growing demand for unified and intelligent revenue cycle platforms across healthcare providers. (Source: https://finthrive.com )
Segments Covered in the Report
By Function
- Medical Coding
- Charge Capture
- Claims Submission
- Payment Posting
- Denial Management
- Accounts Receivable Follow-Up
- Revenue Integrity and Audit
- Contract Management
- Others
By Component
- Software
- Services
By Deployment Mode
- Cloud-based
- On-premise
- Hybrid
By End User
- Hospitals
- Physician Groups
- Ambulatory Surgical Centers
- Diagnostic Laboratories
- Others
By Region
- North America
- Latin America
- Europe
- Asia-pacific
- Middle and East Africa
For inquiries regarding discounts, bulk purchases, or customization requests, please contact us at [email protected]
Frequently Asked Questions
Ask For Sample
No cookie-cutter, only authentic analysis – take the 1st step to become a Precedence Research client
 Get a Sample
Get a Sample
 Table Of Content
Table Of Content




.webp)


 +1 804-441-9344
+1 804-441-9344
 Schedule a Meeting
Schedule a Meeting
