What is AI in Medical Billing Market Size in 2026?
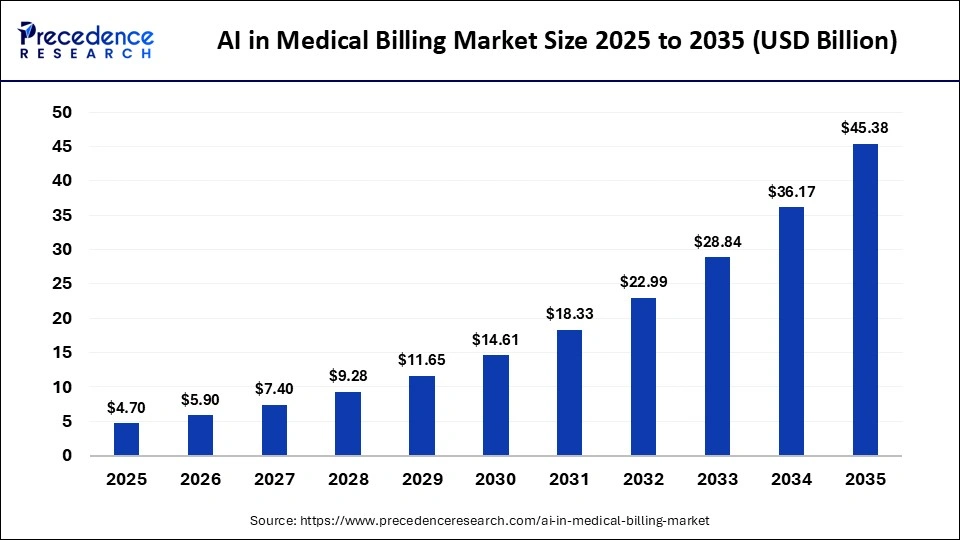
The global AI in medical billing market size was calculated at USD 4.70 billion in 2025 and is predicted to increase from USD 5.90 billion in 2026 to approximately USD 45.38 billion by 2035, expanding at a CAGR of 25.44% from 2026 to 2035. The market is rapidly growing due to rising adoption of AI-driven automation, the growing amount of healthcare data, the need to minimize errors in billing, and the need for faster and more accurate revenue cycle management.
Key Takeaways
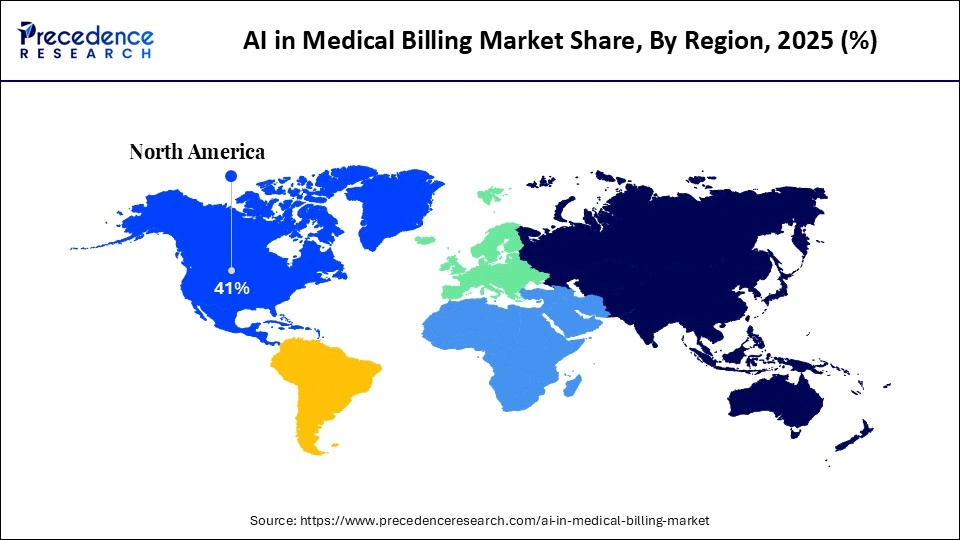
- North America led the AI in medical billing market with the largest share of 41% in the global market in 2025.
- Asia-Pacific is expected to grow at the highest CAGR during the forecast period.
- By offering type, the AI software platforms segment led the market and held approximately 46% share in 2025.
- By offering type, the data analytics and optimization tools segment is expected to grow at the highest CAGR during the forecast period.
- By deployment type, the cloud-based platforms segment dominated the market with approximately 63% share in 2025.
- By deployment type, the hybrid deployments segment is expected to grow at the highest CAGR between 2026 and 2035.
- By technology type, the machine learning segment led the market and captured 41% share in 2025.
- By technology type, the predictive analytics segment is expected to expand at the highest CAGR from 2026 to 2035.
- By end user type, the hospitals and clinics segment led the market with approximately 56% share in 2025.
- By end user type, the billing outsourcing firms segment is expected to expand at the highest CAGR from 2026 to 2035.
What is the AI in Medical Billing Market?
The global AI in medical billing market includes artificial intelligence-powered platforms and services used to automate healthcare billing processes such as medical coding, claim submission, denial management, revenue cycle management (RCM), and payment processing. AI technologies such as machine learning (ML), natural language processing (NLP), and predictive analytics help reduce billing errors, accelerate claims processing, improve compliance, and enhance financial performance for healthcare providers and payers.
Technology Shifts in the AI in Medical Billing Market
The technology trends in the market are heading towards more sophisticated, model-driven, and automated solutions. AI models like deep learning and transformer-based natural language processing(NLP) are being adopted for extracting structured data from clinical notes and associating it with the correct billing codes. There is also a shift towards closed-loop learning systems, where models keep improving based on claim outcomes and denial feedback.
Predictive algorithms are being adopted for risk prediction of denials and optimizing claim submission strategies. The market is shifting towards real-time validation engines for instant validation of claims through low-latency processing engines. The market is becoming more API-centric, facilitating smooth data transfer between billing systems and electronic health records. Unsupervised learning models are being utilized for anomaly detection, which helps in detecting fraud and compliance problems.
AI in Medical Billing Market Trends
- Collaborations and Partnerships: AI technology companies are collaborating with revenue cycle management(RCM) companies to leverage the power of machine learning with billing expertise. These partnerships aim to automate coding, denial prediction, and claims optimization on integrated platforms. For instance, Google Cloud collaborated with IKS Health to build AI agents to optimize coding and prior authorization processes.
- Government Initiatives: Governments are enhancing digital infrastructure in the healthcare sector to facilitate AI-driven administrative systems, such as billing and claims management. Health data platforms and interoperability technology are being developed to provide structured electronic health records. For instance, the National Health Authority of India is promoting digital health adoption through the Ayushman Bharat Digital Mission, providing a foundation for AI-driven healthcare operations.
- Business Expansions: Businesses are expanding their AI-driven billing solutions through acquisitions and product enhancements. Companies are integrating predictive analytics and automation capabilities into comprehensive revenue cycle solutions to enhance efficiency and accuracy. For instance, R1 RCM is expanding its AI solutions to hospital networks to automate claims management and financial operations.
Market Scope
| Report Coverage | Details |
| Market Size in 2025 | USD 4.70 Billion |
| Market Size in 2026 | USD 5.90 Billion |
| Market Size by 2035 | USD 45.38 Billion |
| Market Growth Rate from 2026 to 2035 | CAGR of 25.44% |
| Dominating Region | North America |
| Fastest Growing Region | Asia Pacific |
| Base Year | 2025 |
| Forecast Period | 2026 to 2035 |
| Segments Covered | Offering, Deployment Type, Technology Type, End User Type, and region, |
| Regions Covered | North America, Europe, Asia-Pacific, Latin America, and Middle East & Africa |
Segmental Insights
Offering Type Insights
Why Did the AI Software Platforms Segment Dominate the AI in Medical Billing Market?
The AI software platforms segment dominated the market with approximately 46% share in 2025. The market growth of this segment is because it provides end-to-end automation in a single system for coding, claims processing, and revenue cycle management. The software platforms process large amounts of data with high accuracy and provide functionalities such as real-time claim validation, denial prediction, and automated error detection. The market growth of this segment is further driven by its scalability, standardized processes, and continuous improvement capabilities through machine learning.
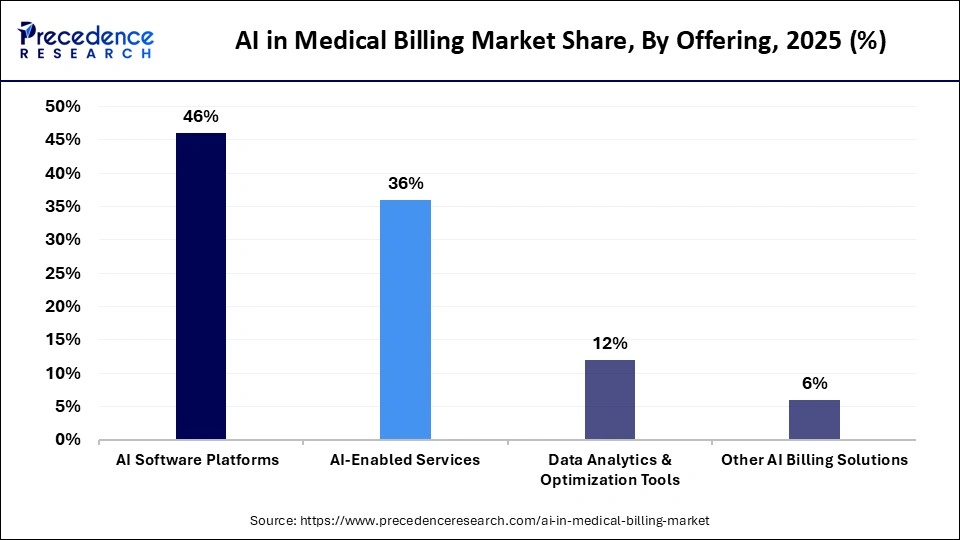
The data analytics and optimization tools segment is expected to grow at the highest CAGR from 2026 to 2035. The market growth of this segment can be attributed to its ability to provide financial and operational insights from billing data. Optimization tools apply advanced analytics and machine learning algorithms to analyze patterns in claims, detect inefficiencies, and point out areas of revenue leakage. Since the billing system produce massive amount of data, healthcare organizations are increasingly turning to analytics tools to make decisions faster and more accurately.
Deployment Type Insights
Why Did the Cloud-Based Platforms Segment Dominate the AI in Medical Billing Market?
The cloud-based platforms segment led the market and held approximately 63% share in 2025. The market growth of this segment can be attributed to greater scalability, flexibility, and cost-effectiveness compared to on-premise solutions. This segment facilitates medical facilities to remotely access medical billing systems, receive real-time updates, and provide smooth integration with other medical technologies. Cloud-based systems manage a substantial amount of data effectively while ensuring automated backups and data management.
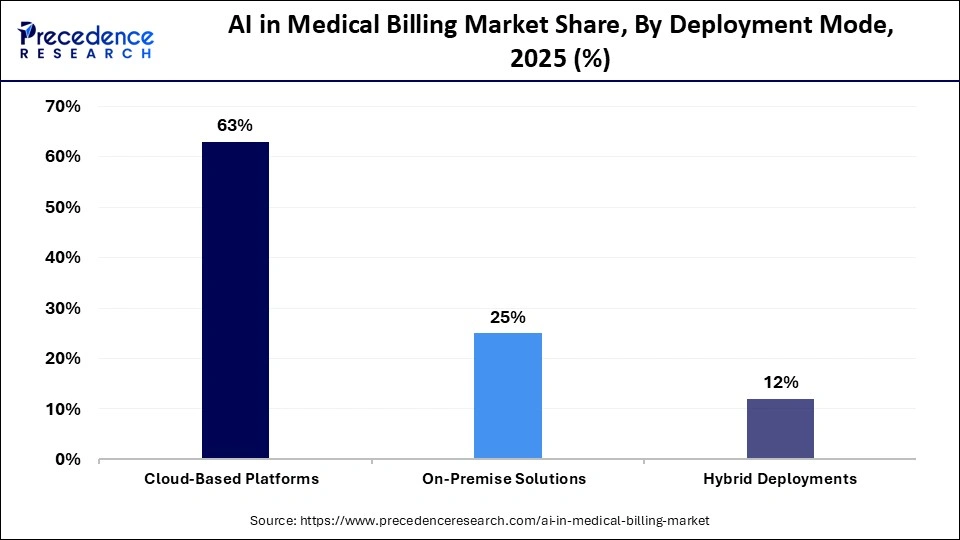
The hybrid deployments segment is expected to grow at the highest CAGR during the forecast period. The market growth of this segment is because it offers the best of both worlds, that is, the control offered by on-premise solutions and the scalability of cloud solutions. Healthcare organizations can store their confidential patient and financial information on-premises while using the cloud for analytics, AI models, and handling large amounts of data. This approach enables organizations to have improved data security and compliance without having to compromise on performance and flexibility.
Technology Type Insights
Why Did the Machine Learning Segment Dominate the AI in Medical Billing Market?
The machine learning segment dominated the market and held approximately 41% share in 2025. The market growth of this segment is because machine learning is the driving force behind most billing automation and decision-making. Machine learning algorithms are capable of processing large amounts of historical claims data to identify patterns and optimize coding accuracy and error detection before claims are submitted. This segment is widely adopted in denial prediction, fraud detection, and reimbursement optimization, where continuous learning from new data improves the machine learning model's performance over time.
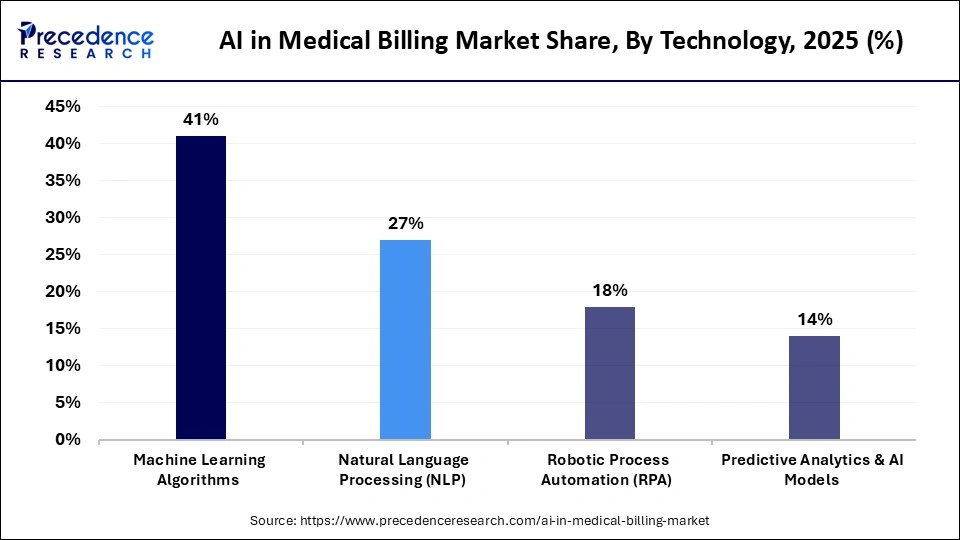
The predictive analytics segment is expected to expand at the highest CAGR during the forecast period. The market growth of this segment is because it facilitates proactive decision-making in billing processes. Predictive models rely on past claims and payment information to predict denial and reimbursement timelines, as well as possible revenue leakage. The capability of predictive analytics in reducing uncertainty and optimizing financial performance is leading to its adoption at a rapid pace.
End User Type Insights
Why Did the Hospitals and Clinics Segment Dominate the AI in Medical Billing Market?
The hospitals and clinics segment dominated the market with approximately 56% share in 2025. The market growth of this segment is because hospitals and clinics have the largest number of patient visits, procedures, and insurance claims. This segment has complex billing cycles with multiple departments. Hospitals and clinics manage the revenue cycle, which is why AI solutions are critical to optimize coding, claim denial, and reimbursement. The market growth of this segment is further driven by its capability to invest in IT infrastructure to support the use of AI-based billing solutions.
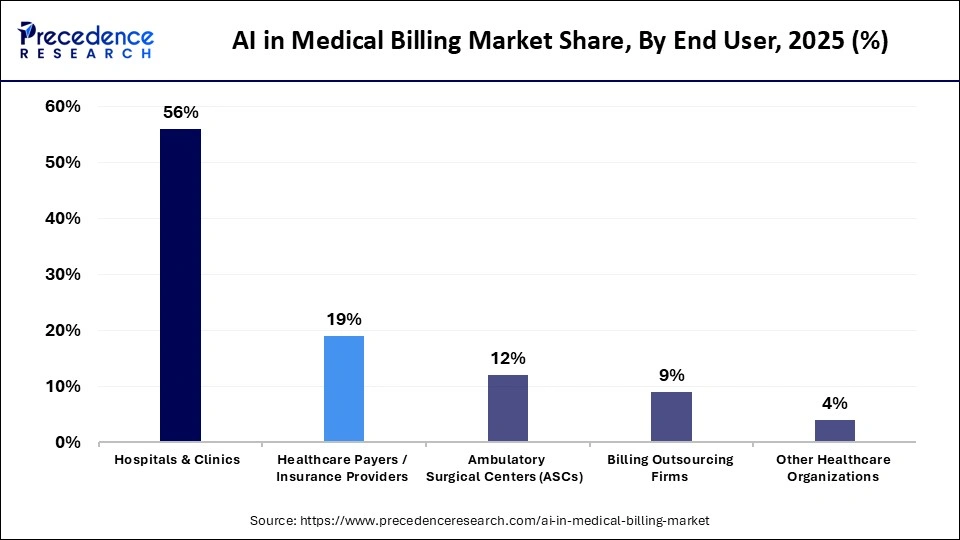
The billing outsourcing firms segment is expected to expand at the highest CAGR during the forecast period. The market growth of this segment is because outsourcing companies are quickly adopting AI technologies to increase efficiency and expand their business with multiple healthcare clients. They process a high volume of claims from various healthcare providers, and AI technology assists in standardizing the process, minimizing errors, and increasing the turnaround time.
Regional Insights
North America AI in Medical Billing Market Size and Growth 2026 to 2035
The North America AI in medical billing market size is estimated at USD 1.93 billion in 2025 and is projected to reach approximately USD 18.83 billion by 2035, with a 25.58% CAGR from 2026 to 2035
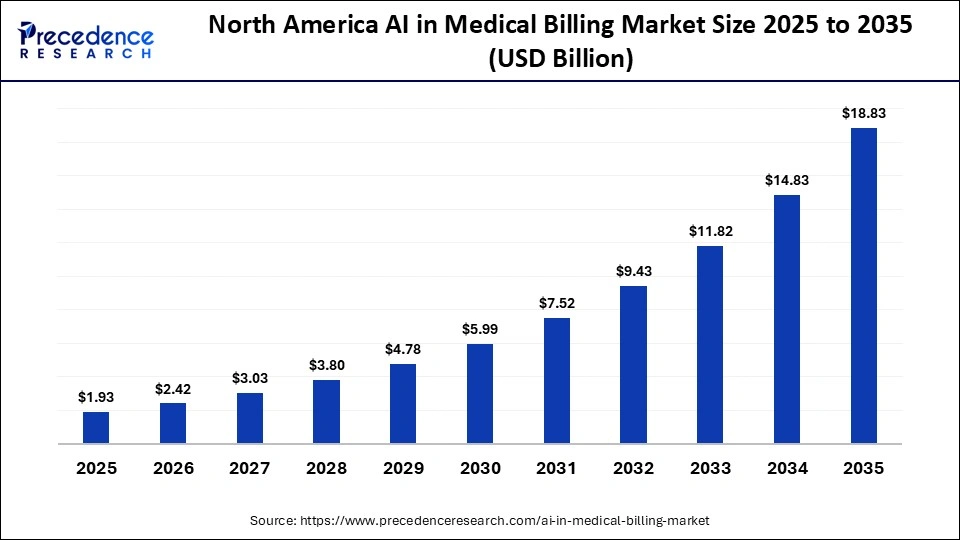
What Made North America the Leading Region in the AI in Medical Billing Market?
North America dominated the AI in Medical Billing market with the largest share of 41% in the global market in 2025. The market growth in this region can be attributed to its advanced healthcare infrastructure and sophisticated insurance billing systems. This region has a large number of claims with stringent coding regulations, thus requiring efficient billing solutions. The healthcare infrastructure in this region is one of the first to adopt cutting-edge AI technology, making it easier to implement AI-based billing solutions. The market growth in this region is further driven by the presence of prominent healthcare IT companies and revenue cycle management firms.
U.S. AI in Medical Billing Market Size and Growth 2026 to 2035
The U.S. AI in medical billing market size is estimated at USD 1.45 billion in 2025 and is projected to reach approximately USD 14.22 billion by 2035, with a 25.65% CAGR from 2026 to 2035.
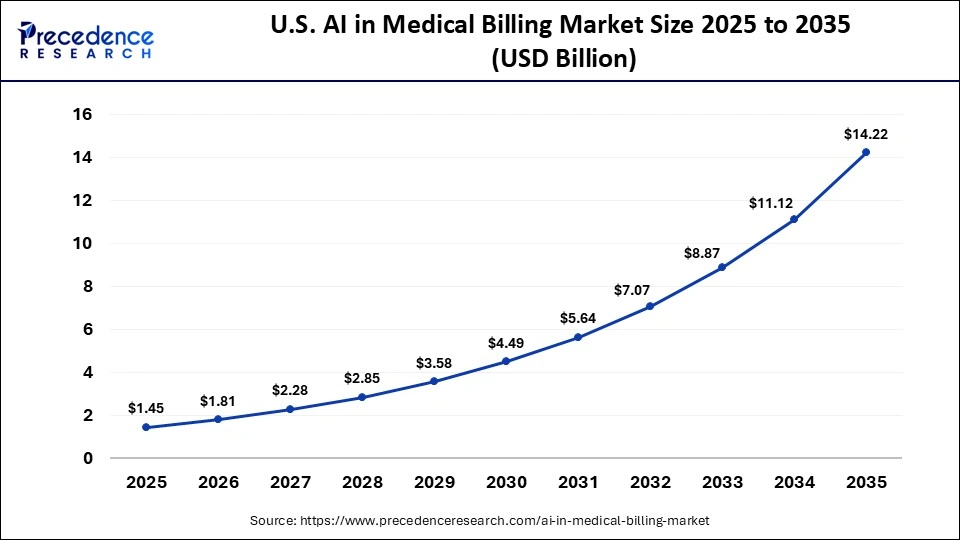
U.S AI in Medical Billing Market Analysis
The U.S. leads the market in North America because of its well-structured billing system and the presence of private insurance companies and healthcare networks. This country has a large number of hospitals, physician practices, and billing companies that produce a huge amount of financial and medical data. The U.S. has a well-established health technology industry with a focus on revenue cycle innovation, as well as the use of standardized coding systems and electronic medical records.
What Made Asia Pacific the Fastest Growing Region in the AI in Medical Billing Market?
Asia Pacific is expected to grow at the highest CAGR from 2026 to 2035. The market growth in this region is due to the rapid development of healthcare infrastructure and the adoption of digital healthcare solutions. This region has a large and growing patient base, resulting in an increased amount of billing data and administrative work. This is the driving need for healthcare providers to implement automated solutions to increase efficiency and accuracy.
China AI in Medical Billing Market Trends
China leads the market in the Asia Pacific because of its widespread adoption of healthcare digitization. This country has rapidly adopted electronic health records and health data platforms, which are ideal for the implementation of AI in administrative tasks such as billing. China is also home to a growing AI and health technology industry that is actively working on developing solutions for hospitals and financial management. The high patient base, infrastructure, and innovation make it easier for the adoption of AI billing systems, making China the leader in the Asia Pacific region.
AI in Medical Billing Market Comapnies
- Waystar
- NextGen Healthcare, Inc.
- McKesson Corporation
- Epic Systems Corporation
- Athenahealth, Inc.
- eClinicalWorks LLC,
- GE Healthcare, Optum, Inc.
- RapidClaims.Ai
- Nym Health
Recent Developments
- In November 2025, Jorie AI showcased SmartCore Engine at HLTH 2025. SmartCore Engine is an AI engine that serves as an intelligent hub that integrates billing systems, payer information, and clinical data. This helps to automate billing processes and optimize claims processing in multi-hospital healthcare systems. (Source: https://www.accessnewswire.com)
- In March 2025, Azalea Health rolled out its AI-powered Billing Assistant, which uses AI to identify common coding errors, alert potential issues, and minimize time spent on correcting claims prior to payment processing. It assists in accelerating approvals and minimizing manual follow-ups in billing processes.
(Source: https://www.azaleahealth.com) - In April 2025, Cedar launched Kora, an AI voice agent that can address patient billing calls 24/7. Kora listens to queries, provides information on bills, and even recommends payment methods. This helps call centers address common billing questions without human assistance.
(Source: https://www.fiercehealthcare.com)
Segments Covered in This Report
By Offering
- AI Software Platforms
- Medical coding automation tools
- Revenue cycle management platforms
- AI-Enabled Services
- Implementation & consulting
- Managed RCM services
- Data Analytics & Optimization Tools
- Other AI Billing Solutions
By Deployment Mode
- Cloud-Based Platforms
- On-Premise Solutions
- Hybrid Deployments
By Technology
- Machine Learning Algorithms
- Natural Language Processing (NLP)
- Robotic Process Automation (RPA)
- Predictive Analytics & AI Models
By End User
- Hospitals & Clinics
- Healthcare Payers / Insurance Providers
- Ambulatory Surgical Centers (ASCs)
- Billing Outsourcing Firms
- Other Healthcare Organizations
By Region
- North America
- Europe
- Asia-Pacific
- Latin America
- Middle East & Africa
For inquiries regarding discounts, bulk purchases, or customization requests, please contact us at sales@precedenceresearch.com
Frequently Asked Questions
Ask For Sample
No cookie-cutter, only authentic analysis – take the 1st step to become a Precedence Research client
 Get a Sample
Get a Sample
 Table Of Content
Table Of Content




.webp)

 sales@precedenceresearch.com
sales@precedenceresearch.com
 +1 804-441-9344
+1 804-441-9344
 Schedule a Meeting
Schedule a Meeting
