Artificial pancreas systems represent a major advancement in diabetes care by enabling automated and adaptive insulin delivery. With the integration of AI, wearable sensors, and digital health platforms, these systems provide more accurate glucose control, reduce complications, and support a more convenient and patient-centric treatment approach.
Abstract
Artificial pancreas device systems (APDS) are novel approaches in the treatment of diabetes mellitus, providing a comprehensive solution to the management of diabetes mellitus, and can be characterized as the combination of continuous glucose monitoring, automated insulin delivery, and intelligent control algorithms. These systems are meant to imitate the workings of a normal pancreas, lessening the burden of manual glucose monitoring and enhancing patient care. Biomedical engineering, data analytics, and new digital health technologies converged to create highly adaptive and accurate systems that can make decisions in real-time. With the growing global burden of diabetes, artificial pancreas systems are becoming a revolution when it comes to optimum glycemic control and improved patient quality of life.
Executive Summary
Artificial pancreas systems are reinventing diabetes management through automation and intelligence in the management of glucose. These systems save a lot of manual intervention, which is necessary, and patients have been able to control their glycaemic status with minimal effort. Hybrid closed-loop systems, combining automation with user input and fully automated systems, are the current and fastest-growing products in the market as the next wave of innovation. Artificial intelligence (AI) has also increased the performance of the system through predictive delivery of insulin and adaptive learning. The rising use of diabetes and the development of wearable medical technology are growing significantly in the face of cost, technical complexity, and regulatory requirements. The future of artificial pancreas systems is full autonomy, better accessibility, and uninterrupted connection to digital health ecosystems.
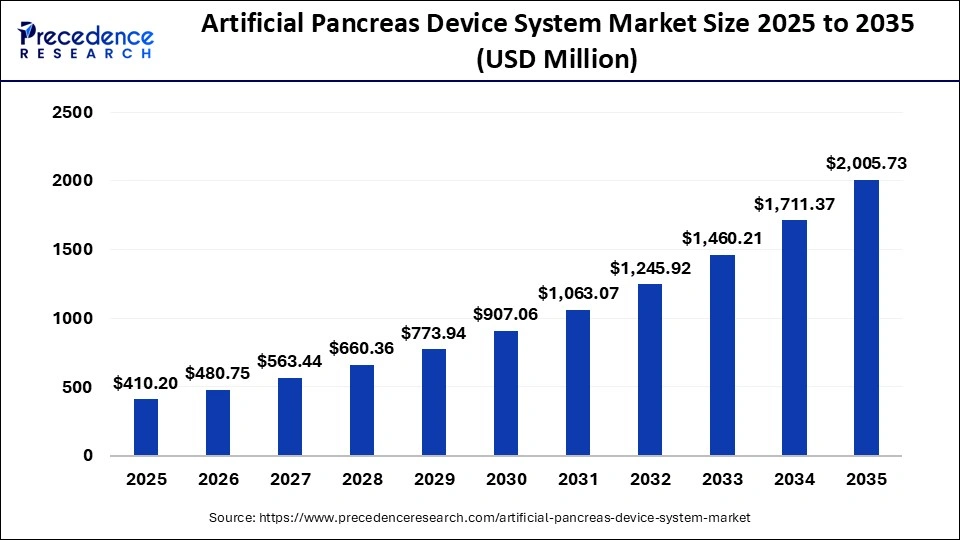
What is the Artificial Pancreas Device System Market Size in 2026?
The global artificial pancreas device system market was valued at USD 410.20 million in 2025 and is projected to grow from USD 480.75 million in 2026 to approximately USD 2,005.73 million by 2035, registering a CAGR of 17.20% from 2026 to 2035. The market is driven by the increasing prevalence of diabetes and the growing demand for advanced solutions that enable accurate, real-time glucose monitoring and automated insulin delivery, replicating natur pancreatic functions.
Get a Free Sample Report with Key Market Trends: https://www.precedenceresearch.com/sample/8214
Unlocking the Power of Persuasion: A Captivating Introduction
Diabetes mellitus is a long-term metabolic disorder, which is defined by the lack of insulin production or its use with the subsequent high level of glucose in the bloodstream. This is physically and psychologically challenging to the patients, who need to monitor and administer insulin on time to prevent improper management. Conventional methods, such as finger-prick tests and multiple daily insulin injections, tend to lead to glucose control variability and a higher risk of complications. Systems of artificial pancreas devices help overcome these drawbacks because they automate the process of insulin delivery and glucose monitoring. These systems offer a more stable and accurate method of managing diabetes by constantly monitoring the level of glucose and making changes to the insulin dosage in real time. The development of artificial pancreas technology is an example of the major innovation efforts in the medical device, software engineering, and data science fields that make it a pillar of present-day, patient-centred healthcare.
Artificial Pancreas System Evolution
In the evolution of artificial pancreatic systems, bigger systems in hospitals have been developed into smaller portable systems, which one can use every day. The initial models were based on manual inputs, but there was a lack of automation, which made them not very practical. With the introduction of continuous glucose monitoring, this has become more reactive as real-time data can be collected and allows for more responsive insulin delivery.
With time, sensor technology has become more accurate and improved with better devices due to advancement in microelectronics. Wireless communication and mobile applications have also been integrated to increase usability, where monitoring and managing diabetes have become better between patients and healthcare providers. Current systems are becoming smarter with machine learning algorithms, which adapt to the needs and behavior of individual patients.
System Architecture and Core Components of Artificial Pancreas Systems
Artificial pancreas systems are sophisticated biomedical systems designed to mimic the glucose-regulating function of a healthy pancreas, utilizing a network of interconnected units that work collaboratively to achieve optimal glucose homeostasis. The main components of these systems include:
- Continuous Glucose Monitoring (CGM) Sensors: CGM sensors play a crucial role in maintaining glucose levels by measuring interstitial glucose concentrations at regular intervals, typically every few minutes. These sensors employ advanced technologies to deliver real-time glucose data, allowing for more responsive management of blood sugar levels. Modern CGMs are known for their high accuracy, which minimizes the risk of incorrect insulin dosing. They have significantly reduced calibration needs, allowing users to rely on them for prolonged periods without frequent adjustments. Many of the latest models also boast extended wear times, improving user convenience and adherence to monitoring protocols.
- Insulin Delivery Devices: Insulin delivery mechanisms, which include insulin pumps or patch systems, are responsible for administering precise amounts of insulin subcutaneously, based on the information received from CGM sensors. These devices are designed to be portable and user-friendly, enabling individuals to manage their diabetes discreetly and effectively. Insulin pumps can provide a continuous basal insulin supply and deliver bolus doses for meals, tailored to the user's specific needs. Patch systems simplify the delivery process even further, offering ease of use without the need for external syringes or vials.
- Control Algorithms: At the heart of an artificial pancreas system lie the control algorithms, which serve as the "brain" of the entire system. These algorithms process incoming glucose data from CGM sensors to determine the optimal insulin dosage to administer. They incorporate advanced predictive modeling and adaptive learning techniques to enhance therapeutic accuracy and personalize treatment to the individual user. By analyzing trends in glucose levels and making real-time adjustments to insulin delivery, these algorithms help maintain glucose levels within a target range, thereby reducing the risk of both hyperglycemia and hypoglycemia. Together, these components create an integrated system that significantly enhances the management of diabetes, providing users with improved quality of life and greater control over their condition.
Artificial Pancreas Systems Classification
Artificial pancreas systems can be classified according to a range of criteria, including their degree of automation and functionality. Hybrid closed-loop systems are the most popular ones nowadays, because they automate the delivery of basal insulin, but the user input is needed to deliver mealtime doses. Such systems offer a balance between automation and control and are therefore applicable to a large proportion of patients.
The further level of innovation is fully closed-loop systems, which do not need any intervention of the user whatsoever. These systems promise real autonomy in diabetes management by constantly changing the amount of insulin delivered according to real-time glucose readings. They are still in their stage of development, but they will enhance better treatment results. Systems that offer both insulin and glucagon (bihormonal) offer further regulation as the high and low blood glucose levels are covered. This dual-hormone method is a closer reflection of the natural pancreatic action and is a promising field of research in the future.
Clinical Outcomes and Benefits to Patients
Artificial pancreas systems have a great clinical benefit over conventional approaches to the treatment of diabetes. These systems lower the risk of both short-term and long-term complications through longer-term glucose level maintenance within a target range. There are reduced instances of hypoglycaemia and hyperglycaemia experienced by patients, and overall health benefits are realized. Besides clinical advantages, they can improve patient convenience and quality of life by minimizing the necessity to constantly monitor patients and administer insulin manually. Their increased adoption is also enhanced by improved adherence to treatment and less psychological load.
Digital Health Ecosystems Integration.
Introduction of artificial pancreas ecosystems into digital health technologies is turning the management of diabetes into a more interactive and active process. There is an opportunity to monitor the level of glucose, set up alerts, and adjust settings in real time with the help of mobile applications. Patient data is available remotely, which enables healthcare providers to monitor patients and provide tailored care. This connection is in line with the wider trend of telemedicine and remote healthcare, especially in the areas that are poorly served by specialized medical care. Artificial pancreatic systems are emerging as part of a modern healthcare system as they allow unhindered flow of information between patients and providers.
Market Environment and Industry Trends
The market for artificial pancreas device systems is characterized by rapid technological advancements and intensifying competition among key players in the industry. This dynamic landscape is largely driven by a significant rise in the prevalence of diabetes globally, along with a growing public awareness regarding innovative treatment options that aim to manage this chronic condition more effectively. As a result, there is an increasing demand for artificial pancreas systems, which provide automated insulin delivery solutions that can enhance patient quality of life and better control blood glucose levels. To capitalize on this burgeoning market, companies are investing substantial resources in research and development (R&D) initiatives. This investment is focused on enhancing product functionality, improving insulin delivery precision, and ensuring user-friendliness, which are critical to capturing a larger market share. Additionally, the integration of cutting-edge technologies in device manufacturing is transforming traditional approaches to diabetes management.
Strategic partnerships and collaborations play a pivotal role in this industry, as firms seek to accelerate innovation and bring advanced products to market more efficiently. By working alongside experts in fields such as medical devices, software engineering, and data analytics, industry players can develop more sophisticated solutions that incorporate real-time data monitoring and machine learning algorithms. This collaborative approach not only fosters technological advancement but also enables the creation of tailored solutions that meet the diverse needs of patients and healthcare providers.
Hybrid Closed-Loop Insulin Pump System
A hybrid closed-loop insulin pump system is a sophisticated system for diabetes management that develops a system to automate the delivery of insulin, although it is still possible to provide user input to the device when needed, especially regarding the mealtime dose. This system is sometimes called a semi-automated artificial pancreas and is a single system that comprises a CGM, an insulin pump, and a control algorithm that keeps the level of blood glucose in the desired range. It would be a considerable advancement over the conventional insulin treatment by making it less demanding in terms of manual monitoring and manipulation.
The main part of the device is the CGM, which controls the level of glucose in real time and sends the information to the insulin pump. These readings are put through the embedded control algorithm and automatically control the basal (background) insulin delivery in response to increasing or decreasing glucose concentrations. This feedback cycle enables the system to adjust on a regular and small basis all day and night, enhancing the overall glycemic control.
Although it is an automated system, the system is referred to as a hybrid system as it still involves the user to carry out some of its tasks. Patients are required to enter their carbohydrate intake on their own and administer a bolus of insulin with meals. This combination method is safe and flexible because meal-related glucose spikes are not identical, and they might need a specific dosing choice.
The main benefits of a hybrid closed-loop system are the possibility to extend time in range, the period during which the level of glucose in a patient is within the recommended range. These systems ensure that the risks of hypoglycemia and hyperglycemia are minimized by automatically adjusting the application of insulin. They especially work well during the night, when only manual monitoring can be done, and there is a higher probability of not noticing that the hypoglycaemia has been undetected.
In a technological sense, hybrid closed-loop systems are based on complex algorithms that include predictive modelling. These algorithms can study the patterns of glucose levels and predict changes, which can be corrected before it is too late. With time, certain systems may be able to adjust to the specifics of each patient, improving personalization and treatment results.
Hybrid closed-loop systems adoption is increasing gradually because of their clinical utility and convenience. They are highly prescribed to patients with Type 1 and are being applied more frequently in insulin-dependent Type 2 diabetes. Nonetheless, other issues, including the price of the devices, frequent calibration of the sensors, and the necessity of training the users, are also significant points to consider.
Future Projections and Future Innovations
The future of artificial pancreas systems lies in the direction of full automation, higher accuracy, and better user experience. Innovation is predicted to come because of sensor technology, algorithm development, and miniaturization of devices. Closely looped systems with less or no human intervention will become the new standard of care.
The future of artificial pancreatic systems and their integration with other, more expansive digital health platforms will only increase their usefulness and accessibility. These systems will continue to expand with the introduction of newer technologies, including more advanced analytics and next-generation wearable devices. With the advancement of research, artificial pancreas systems are likely to become more central to the management of diabetes globally.
Conclusion
Artificial pancreas device systems are a trailblazing breakthrough in diabetes management, providing a more accurate, computerized, and personalized system of glucose control. These systems are transforming the nature of treatment by incorporating continuous monitoring, smart algorithms, and automatic delivery of insulin. With the ongoing trend in technological innovation and the subsequent removal of obstacles to its actualization, artificial pancreas systems can become highly accessible and a standard part of the modern health care system. The fact that they can enhance clinical outcomes, increase quality of life, and decrease the burden of disease underscores their importance in the future of managing diabetes.
Expert Advise
According to Precedence Research, the demand for artificial pancreas systems is rapidly rising, with the increasing prevalence of diabetes, advancements in medical technology, and the need to monitor insulin levels. The artificial pancreas device system industry is evolving rapidly, as stakeholders aim to deliver more intelligent and convenient diabetes management solutions, ultimately enhancing treatment outcomes for patients and positioning themselves competitively within the healthcare landscape.
About the Authors

Aditi Shivarkar
Aditi, Vice President at Precedence Research, brings over 15 years of expertise at the intersection of technology, innovation, and strategic market intelligence. A visionary leader, she excels in transforming complex data into actionable insights that empower businesses to thrive in dynamic markets. Her leadership combines analytical precision with forward-thinking strategy, driving measurable growth, competitive advantage, and lasting impact across industries.

Aman Singh
Aman Singh with over 13 years of progressive expertise at the intersection of technology, innovation, and strategic market intelligence, Aman Singh stands as a leading authority in global research and consulting. Renowned for his ability to decode complex technological transformations, he provides forward-looking insights that drive strategic decision-making. At Precedence Research, Aman leads a global team of analysts, fostering a culture of research excellence, analytical precision, and visionary thinking.

Piyush Pawar
Piyush Pawar brings over a decade of experience as Senior Manager, Sales & Business Growth, acting as the essential liaison between clients and our research authors. He translates sophisticated insights into practical strategies, ensuring client objectives are met with precision. Piyush’s expertise in market dynamics, relationship management, and strategic execution enables organizations to leverage intelligence effectively, achieving operational excellence, innovation, and sustained growth.





 Request Consultation
Request Consultation

