What is the AI for Healthcare Payer Market Size in 2026?
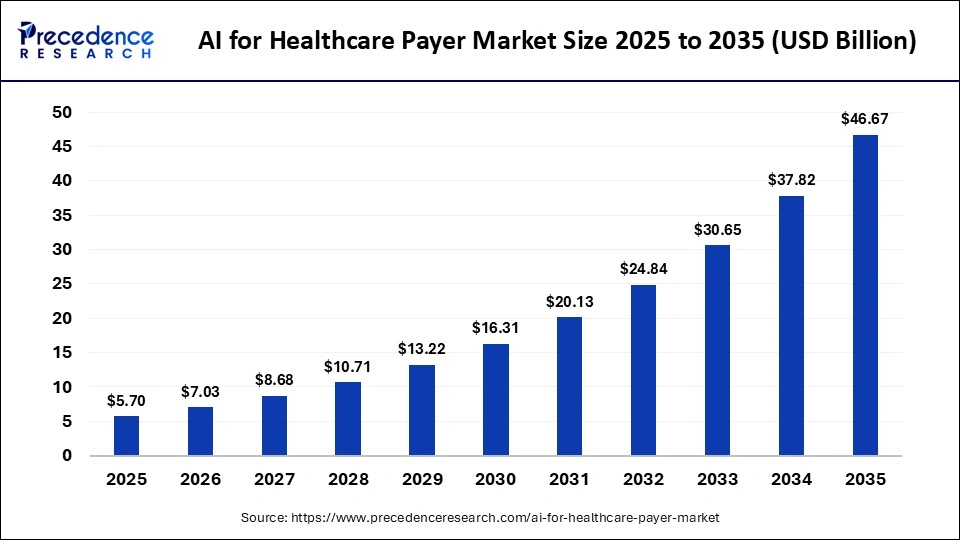
The global AI for healthcare payer market size accounted for USD 5.70 billion in 2025 and is predicted to increase from USD 7.03 billion in 2026 to approximately USD 46.67 billion by 2035, expanding at a CAGR of 23.40% from 2026 to 2035. The market is rapidly expanding due to the increased adoption of cloud-based AI platforms in the healthcare industry, rising demand for value-based care services, and the need to achieve administrative work efficiency with evolving technologies like AI/ML and NLP.
Key Takeaways
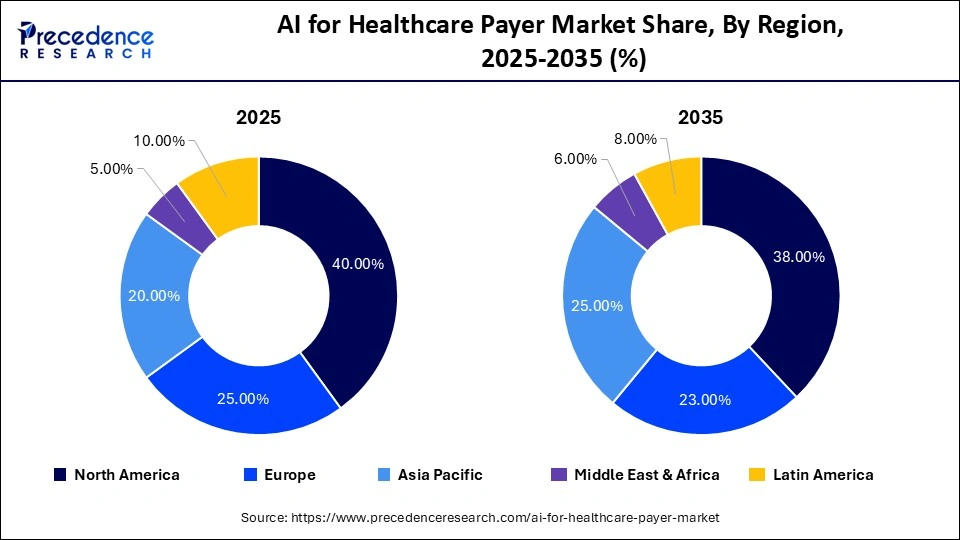
- North America held the largest share of 40% in the AI for healthcare payer market in 2025.
- Asia Pacific is expected to grow at the fastest CAGR of 26% during the forecast period of 2026-2035.
- By technology, the machine learning (ML) & deep learning (DL) segment held the largest market share of 35% in 2025.
- By technology, the natural language processing (NLP) segment is the second-largest shareholder and is expected to grow at a CAGR of 20% during the forecast period.
- By application, the claims processing & management segment held the largest market share of 30% in 2025.
- By application, the fraud detection & risk management segment is the second-largest shareholder and is expected to grow at a CAGR of 23.5% during the forecast period.
- By deployment mode, the cloud-based AI solutions segment held the largest market share of 60% in 2025.
- By deployment mode, the on-premises AI solutions segment is the second-largest shareholder and is expected to grow at a CAGR of 17.5% during the projection period.
- By end-use, the private health insurers segment held the largest market share of 50% in 2025.
- By end-use, the public health insurers segment is the second-largest shareholder and is expected to grow at the fastest CAGR of 23.5% between 2026 and 2035.
Market Overview
AI for healthcare payers refers to the application of cutting-edge technologies like machine learning, generative AI, and natural language processing to automate, streamline, and optimize administrative and clinical operations of companies providing health insurance. The AI for healthcare payer market is rapidly growing due to the increasing demand for administrative work efficiency with cost reduction, to increase member engagement and personalization, and to detect potential fraud.
Leading payers are collaborating with giant tech companies like Google Cloud, Microsoft, and Cognizant to deploy AI-powered platforms aiming to streamline payment processes and enhance services for members. The increasing data generation in healthcare from electronic health records, wearable devices, and internet of medical things devices offers the required data for training AI models and deriving actionable insights.
AI for Healthcare Payer Market Trends
- Many payers are increasingly leveraging generative AI and large language models to automate repetitive administrative tasks and reduce operational burdens. These applications include claims processing, appeal management, and prior authorization reviews.
- There is a rapid shift toward more autonomous healthcare operations powered by agentic AI systems. Unlike traditional rule-based chatbots, these advanced systems can proactively manage member interactions and workflows with minimal human intervention, improving efficiency and responsiveness.
- Payers are investing in AI-enabled virtual assistants as part of broader digital front door strategies. These platforms enhance member engagement by providing transparent pricing information, personalized support, and 24/7 service availability, ultimately improving customer retention.
- Machine learning algorithms are also being deployed to analyze claims data and detect anomalies such as upcoding and unbundling before payments are made. This helps improve overall payment integrity.
Market Scope
| Report Coverage | Details |
| Market Size in 2025 | USD 5.70 Billion |
| Market Size in 2026 | USD 7.03 Billion |
| Market Size by 2035 | USD 46.67 Billion |
| Market Growth Rate from 2026 to 2035 | CAGR of 23.40% |
| Dominating Region | North America |
| Fastest Growing Region | Asia Pacific |
| Base Year | 2025 |
| Forecast Period | 2026 to 2035 |
| Segments Covered | Technology, Application, Deployment Mode, End-Use, and Region |
| Regions Covered | North America, Europe, Asia-Pacific, Latin America, and Middle East & Africa |
Market Dynamics
Drivers
Increasing Claim Inaccuracies and Fraudulent Activities
The AI for healthcare payer market is mainly driven by the strong focus of payers on lowering operational costs and reducing false claim cases. It is nearly impossible to precisely find inaccuracies with human efforts due to the vast amount of data generated in the healthcare sector. Therefore, to reduce billing errors and false claims, payers are adopting AI tools to automate tasks like claims processing, prior authorization, and detect anomalies in real-time, which eventually reduces operational costs.
Restraint
Growing Security Concerns
Despite having several benefits, the lack of transparency and security concerns associated with using AI solutions restrain the AI for healthcare payer market. A profound gap still exists where AI is deployed faster than an oversight framework, which creates room for false claims and prior authorization. Stringent regulatory requirements and the complexity of integrating AI with legacy systems pose challenges, particularly for small and medium-sized enterprises with limited budgets and technical resources. As a result, many payers remain cautious about adopting full-scale, enterprise-wide AI implementations. However, as AI technologies mature and regulatory frameworks evolve, these challenges are expected to gradually ease over the forecast period.
Opportunity
Rise of Agentic AI
The rise of agentic AI creates immense opportunities in the AI for healthcare payer market. AI agents can work independently without human interruption and are able to interpret medical policies, navigate rules of payers, create summaries, and resubmit claims or prior authorization autonomously. These systems improve self-learning and accelerate processes by reducing burnout across administrative teams. Therefore, health systems and health payers are rapidly moving toward AI-curated and real-time clinical data exchange, creating massive growth opportunities for the market.
Segment Insights
Technology Insights
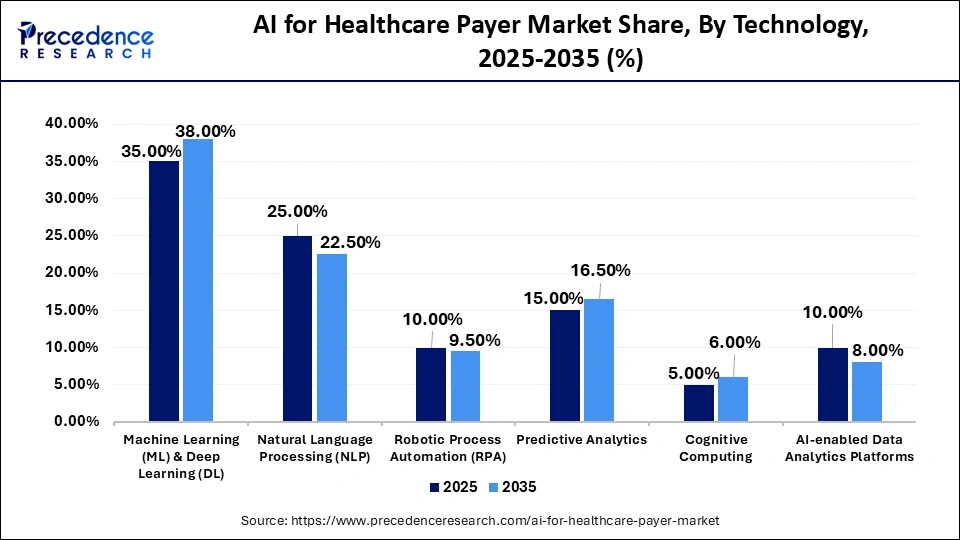
AI for Healthcare Payer Market Share, By Technology, 2025-2035 (%)
| Technology | 2025 | 2035 | CAGR (%) |
| Machine Learning (ML) & Deep Learning (DL) | 35.00% | 38.00% | 24.50% |
| Natural Language Processing (NLP) | 25.00% | 22.50% | 20.00% |
| Robotic Process Automation (RPA) | 10.00% | 9.50% | 19.00% |
| Predictive Analytics | 15.00% | 16.50% | 25.00% |
| Cognitive Computing | 5.00% | 6.00% | 22.00% |
| AI-enabled Data Analytics Platforms | 10.00% | 8.00% | 18.50% |
The ML & DL Segment Held a 35% Market Share in 2025
The machine learning (ML) & deep learning (DL) segment dominated the AI for healthcare payer market with a 35% share in 2025. The segment's dominance is attributed to the ability of ML & DL to analyze huge amounts of healthcare datasets and automate decision-making. These technologies further enhance precision in claim management and fraud detection systems, making them the preferred choice.
The natural language processing (NLP) segment was the second-largest shareholder in 2025, holding a 25% share, and is expected to grow at a CAGR of 20% during the forecast period. The segment growth is driven by the crucial role played by NLP technology to extract insights from unstructured data like medical records and insurance claims. It enhances patient engagement and administrative processes.
The robotic process automation (RPA) segment held the market share of 10% in 2025 and is expected to grow at a CAGR of 19% during the projection period. This is because robotic process automation is increasingly used to automate repetitive tasks, including claims processing. It further helps reduce operational costs and increases efficiency in payer operations.
The predictive analytics segment held the market share of 15% in 2025 and is expected to grow at the highest CAGR of 25% during the forecasted years of 2026-2035. The segment is largely driven by the increasing need to forecast patient care costs, manage medical claims, and prevent potentially fraudulent activities.
Application Insights
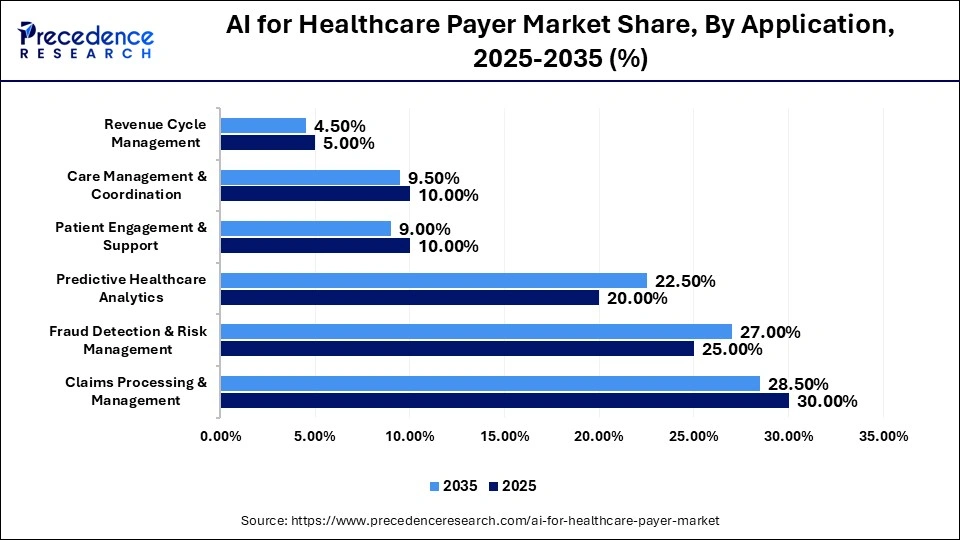
AI for Healthcare Payer Market Share, By Application, 2025-2035 (%)
| Application | 2025 | 2035 | CAGR (%) |
| Claims Processing & Management | 30.00% | 28.50% | 22.00% |
| Fraud Detection & Risk Management | 25.00% | 27.00% | 23.50% |
| Predictive Healthcare Analytics | 20.00% | 22.50% | 25.00% |
| Patient Engagement & Support | 10.00% | 9.00% | 19.00% |
| Care Management & Coordination | 10.00% | 9.50% | 18.50% |
| Revenue Cycle Management | 5.00% | 4.50% | 17.50% |
The Claims Processing & Management Segment Held the Market Share of 25% in 2025
The claims processing & management segment dominated the AI for healthcare payer market while holding a 25% share in 2025. The segment dominance is attributed to its ability to streamline workflows for claims processing and automate administrative tasks. AI integration with claims processing is proven to reduce processing time, operational costs, and enhance accuracy.
The fraud detection & risk management segment held the second-largest market share of 25% in 2025 and is expected to grow at a CAGR of 23.5% during the forecast period. The segment is expanding as AI algorithms help identify suspicious activities, patterns, and inconsistencies in claims. Fraud detection and risk management are highly crucial to reducing financial losses.
The predictive healthcare analytics segment held the market share of 20% in 2025 and is expected to grow at the highest CAGR of 25% in the foreseeable period. The segment is majorly driven by its ability to forecast healthcare costs that assist health payers for further claim processing. By analyzing historical data, it further manages risks and plans for future healthcare demands.
The patient engagement & support segment held the market share of 10% in 2025 and is projected to grow at a CAGR of 19% in the upcoming period. The segment is growing as AI integration helps improve patient engagement and keep the retention rate strong. It offers personalized care plans, real-time support, and enhances overall customer service for health insurers.
Deployment Mode Insights
Why Did the Cloud-Based AI Solutions Segment Dominate the Market in 2025?
The cloud-based solutions segment dominated the AI for healthcare payer market with the highest share of 60% in 2025. The segment's dominance is driven by the ability of this deployment to provide higher scalability and minimize upfront costs. Cloud-based solutions enable access to data and services remotely, making them the preferred choice. They also eliminate the need to visit clinics for better treatment and consultation from healthcare professionals.
AI for Healthcare Payer Market Share, By Deployment Mode, 2025-2035 (%)
| Deployment Mode | 2025 | 2035 | CAGR (%) |
| Cloud-based AI Solutions | 60.00% | 65.00% | 25.00% |
| On-premise AI Solutions | 30.00% | 25.00% | 17.50% |
| Hybrid AI Solutions | 10.00% | 10.00% | 20.00% |
The on-premises AI solutions segment held the second-largest market share of 30% in 2025 and is expected to grow at a CAGR of 17.5% during the forecast period. The segment growth is driven by the increasing demand to secure organizational data and prohibit sharing even with third-party vendors for maximum data protection. On-premises solutions are adopted by many organizations to comply with strict data privacy regulations.
The hybrid AI solutions segment held the market share of 10% in 2025 and is expected to grow at a CAGR of 20% in the upcoming period. This is because of the unmatched flexibility hybrid AI solutions offer. They combine the benefits of cloud deployment and on-premises systems with maximum data privacy to meet the various requirements of different clients.
End-Use Insights
Private Health Insurers Held the Largest Market Share of 50% in 2025
The private health insurers segment dominated the AI for healthcare payer market with the largest share of 50% in 2025. The segment dominance is attributed to the increasing adoption of AI-based solutions by private health insurers. These solutions help them to optimize claims processing, customer services, and enhance operational efficiency as well.
The public health insurers segment held the second-largest share of 25% in 2025 and is expected to grow at the fastest CAGR of 23.5% during the forecast period. The segment is expanding as public health insurers are embracing AI systems to manage healthcare costs and detect fraud. It enhances member engagement and service delivery, supporting the segment growth further.
AI for Healthcare Payer Market Share, By End-Use, 2025-2035 (%)
| End-Use | 2025 | 2035 | CAGR (%) |
| Private Health Insurers | 50.00% | 48.00% | 21.00% |
| Public Health Insurers | 25.00% | 27.00% | 23.50% |
| Third-Party Administrators (TPAs) | 15.00% | 14.00% | 18.50% |
| Health Maintenance Organizations (HMOs) | 10.00% | 11.00% | 20.00% |
The third-party administrators segment held the market share of 15% in 2025 and is expected to grow at a CAGR of 18.5% during the foreseeable period of 2026-2035. The segment is growing as third-party administrators are increasingly leveraging AI technologies to manage claims and billing. It assists in regulatory compliance for health insurers.
The health maintenance organizations (HMOs) segment held the market share of 10% in 2025 and is projected to grow at a CAGR of 20% during the foreseeable period. The segment is growing as HMOs are increasingly adopting AI to improve care management, reduce costs, and ensure high-quality patient care in a managed environment.
Regional Insights
North America AI for Healthcare Payer Market Size and Growth 2026 to 2035
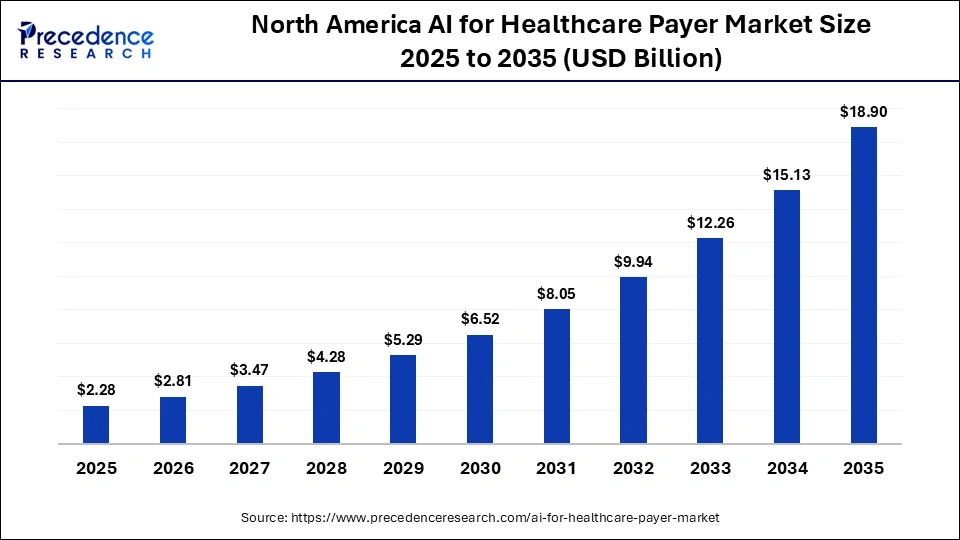
The North America AI for healthcare payer market size is estimated at USD 2.28 billion in 2025 and is projected to reach approximately USD 18.90 billion by 2035, with a 23.55% CAGR from 2026 to 2035.
Why Did North America Lead the AI for Healthcare Payer Market in 2025?
North America dominated the AI for healthcare payer market with the largest share of 40% in 2025. This leadership is driven by the high complexity of administrative healthcare processes, increasing cost pressures, and a robust technological infrastructure that supports the seamless integration of emerging AI solutions. Strong government initiatives, along with significant investments from technology companies, further accelerate market growth in the region.
According to the source, over 80% of healthcare institutions in North America have adopted cloud-based electronic health record (EHR) systems, enabling AI applications to process and analyze large volumes of patient data in real time. The region is also undergoing a transition from fee-for-service models to value-based care, which increases the need for advanced AI tools to measure care efficiency, manage population health, and predict patient risk. Moreover, North America benefits from a strong venture capital ecosystem and substantial R&D investment in healthcare AI, further reinforcing its dominant market position.
U.S. AI for Healthcare Payer Market Size and Growth 2026 to 2035
The U.S. AI for healthcare payer market size is calculated at USD 1.71 billion in 2025 and is expected to reach nearly USD 14.27 billion in 2035, accelerating at a strong CAGR of 23.64% between 2026 and 2035.
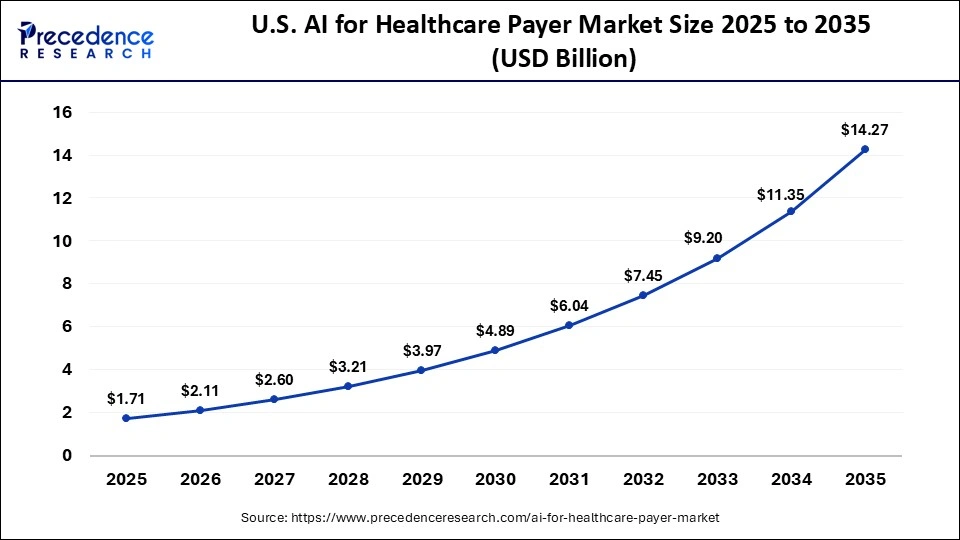
U.S. AI for Healthcare Payer Market Analysis
The U.S. is a major contributor to the market, as it is an early adopter of AI in the healthcare sector due to the favorable regulatory environment. The country is home to tech giants like Microsoft, Oracle, Google, and NVIDIA, which ensure constant innovative capabilities for AI integration. Regulatory support from the U.S. Food and Drug Administration, including initiatives such as the Digital Health Innovation Action Plan, has created structured pathways for the approval and adoption of AI-powered medical technologies.
In addition, U.S. payers are increasingly integrating with provider networks to form payer-provider collaborative models. These models enhance data sharing and enable more effective use of AI for coordinated care delivery, improved decision-making, and better health outcomes.
How is the Opportunistic Rise of Asia Pacific in the AI for Healthcare Payer Market?
Asia Pacific is expected to grow at the fastest CAGR of 26% during the forecast period, driven by a rapidly ageing population seeking cost-effective solutions for managing chronic diseases. Increasing healthcare demands are encouraging payers to adopt AI solutions that enable early engagement with policyholders, helping reduce hospital readmissions and support more cost-efficient care delivery. Healthcare payers across the region are experiencing a rising volume of health insurance claims, driven by increasing insurance penetration, particularly in developing economies. This expansion is further accelerating the adoption of AI-powered systems to improve claims processing efficiency and risk management.
China AI for Healthcare Payer Market Analysis
China is a leading adopter of AI in the healthcare payer sector, driven by its large, centralized healthcare datasets, rapid integration of AI into telemedicine platforms, and strong government support for digital health transformation. National policies such as the New Generation Artificial Intelligence Development Plan prioritize the use of AI in healthcare and provide significant support and incentives for companies developing AI solutions for hospital workflows.
AI for Healthcare Payer Market Companies
- IBM Watson Health
- Optum (UnitedHealth Group)
- Cigna Corporation
- Change Healthcare Inc.
- Cerner Corporation
- McKesson Corporation
- Anthem, Inc.
- Cognizant Technology Solutions Corporation
- NVIDIA Corporation
- SAS Institute Inc.
- Medtronic plc
- Qualcomm Life, Inc.
- GE Healthcare
- CloudMedx
- Palantir Technologies
Recent Developments
- In March 2026, Amazon introduced a health AI agent on its website and app with 24/7 access to virtual care for Prime members. It offer personalized health insights and guidance to take meaningful actions like booking appointments with healthcare professionals.(Source: https://www.aboutamazon.com)
- In February 2026, a global frontrunner in agentic automation, UiPath, announced a new agentic AI solution for the healthcare sector, especially for providers and payers at the ViVE 2026 conference. Agentic automation is being leveraged for medical records summarization, claim denial prevention, and resolution.(Source: https://ir.uipath.com)
- In October 2025, the healthcare AI platform company, Innovaccer Inc, announced the launch of ‘Galaxy by Innovaccer.' It is an integrated and AI-driven platform that transforms how payers manage risk adjustments across value-based care and fee-for-service models.(Source: https://innovaccer.com)
Segments Covered in the Report
By Technology
- Machine Learning (ML) & Deep Learning (DL)
- Natural Language Processing (NLP)
- Robotic Process Automation (RPA)
- Predictive Analytics
- Cognitive Computing
- AI-enabled Data Analytics Platforms
By Application
- Claims Processing & Management
- Fraud Detection & Risk Management
- Predictive Healthcare Analytics
- Patient Engagement & Support
- Care Management & Coordination
- Revenue Cycle Management
By Deployment Mode
- Cloud-based AI Solutions
- On-premises AI Solutions
By End-Use
- Private Health Insurers
- Public Health Insurers
- Third-Party Administrators (TPAs)
- Health Maintenance Organizations (HMOs)
By Region
- North America
- Latin America
- Europe
- Asia-pacific
- Middle and East Africa
For inquiries regarding discounts, bulk purchases, or customization requests, please contact us at sales@precedenceresearch.com
Frequently Asked Questions
Ask For Sample
No cookie-cutter, only authentic analysis – take the 1st step to become a Precedence Research client
 Get a Sample
Get a Sample
 Table Of Content
Table Of Content






 sales@precedenceresearch.com
sales@precedenceresearch.com
 +1 804-441-9344
+1 804-441-9344
 Schedule a Meeting
Schedule a Meeting
